IJCRR - 2nd Wave of COVID-19: Role of Social Awareness, Health and Technology Sector, June, 2021
Pages: 101-104
Date of Publication: 11-Jun-2021
Print Article
Download XML Download PDF
Prevalence of Psychological Distress Among Undergraduate Medical Students During the Covid 19 Pandemic and Their Perception of the Influence of the Pandemic on Their Academics
Author: Chandra Subhash, KP Lakshmi
Category: Healthcare
Abstract:Background: Undergraduate medical students have been affected by the COVID 19 pandemic and are under psychological distress. Objective: To assess the prevalence of psychological distress among MBBS students using the K10 questionnaire and to assess the influence of the COVID 19 pandemic on the perception of the students on how it has affected their academic activities and skills Methods: The study design was a cross-sectional observational study. A two-section questionnaire was sent to MBBS students of all five years studying currently in the institution. The first section: K10 Questionnaire to assess psychological distress and the second: assess the perception of the MBBS students on how the pandemic has influenced their skills and academics. Participation in the study was voluntary. Results: Among 123 students who participated prevalence of psychological distress was 67.5 % (n=83). The mean K10 score was 24.46\?7.91. 33.3 % of the students had severe psychological distress. 82 % of the students had a perception of reduced clinical skills due to the lockdown and 66 % felt that the pandemic would lead to an extension of their courses. Conclusion: There is a high prevalence of psychological distress among medical undergraduate students during the pandemic. There is an increased perception of reduced clinical skills and possible course extension among undergraduate students.
Keywords: COVID19, K10 score, Psychological distress, Clinical skills, Undergraduate students
Full Text:
Introduction
An outbreak of pneumonia of unknown aetiology, which was identified first at Wuhan city in Hubei province of China in December 2019, was caused by a new strain of coronavirus named as 2019 novel coronavirus (2019-nCoV) or SARS-CoV 2.1 This virus rapidly spread across the globe, and subsequently a pandemic was declared on March 11, 2020.2 Since its global recognition, the novel coronavirus disease (COVID-19) pandemic has spread to over 200 countries in less than five months.3 In India, the first case of COVID-19 was reported on January 30, 2020.4 As of February 7, 2021, 10,827,314 laboratory-confirmed cases and 1,55,032 deaths were reported from India. The case reporting is based on the testing of individuals by real-time reverse transcription-polymerase chain reaction (RT-qPCR).5 It is performed by taking nasopharyngeal swabs or throat swab or saliva. A range of RNA target gene is used for detection by different manufacturers, mostly targeting the envelope (E), nucleo-capsid (N), spike (S), RNA-dependent RNA polymerase (RdRp), and ORF1 (Open reading frame)genes.6
In COVID-19 infected symptomatic individuals, viral load can be detected early from day one of symptoms and it peaks within the first seven days of onset of symptoms. This viral load can be measured by the cycle threshold (Ct) value, which is the number of replication cycles required to produce a fluorescent signal. Thus lower Ct values representing higher viral RNA loads. The positivity of the samples starts to decline by 3rd week and subsequently becomes undetectable.6 If only one SARS CoV-2 target gene is detected in the test (multiplex SARS CoV-2 RT PCR test) with valid internal control, the result should be interpreted as Inconclusive and repeated the test.7 Inconclusive SARS CoV-2 reverse transcription-polymerase chain reaction (RT-PCR) reports for the detection of infection in symptomatic patients or during the screening of asymptomatic contacts can cause clinical, diagnostic and infection control uncertainty.8
This study aims to analyze inconclusive results of samples tested at our Centre based on Ct value, duration of symptoms at the time of testing and the results of repeat testing.
Materials and Methods
The study was carried out over 94,443 suspected symptomatic COVID 19 patients as well as asymptomatic groups, such as high-risk contacts or high-risk healthcare workers, as per ICMR guideline9 from June 2020 to December 2020 at COVID laboratory in the Department of Microbiology of Nil Ratan Sircar Medical College & Hospital, Kolkata.
Sample collection & transport
Nasopharyngeal swab and throat swab were collected in Viral transport media from suspected cases in different wards and designated COVID wards of NRS Medical College & Hospital as per ICMR guidelines10 and sent to our Laboratory.
Samples from other district and rural hospitals were also sent to our laboratory as stated by the West Bengal Department of Health and Family Welfare updated from time to time.
Testing and collection of Data
All the samples were processed in our Laboratory as per standard protocol and tested by quantitative reverse transcriptase PCR test with the kits supplied by ICMR and the state Health Department. Results were analyzed thereafter and all data were collected.
Results
A total of 94,443 samples were tested in the COVID laboratory of Nil Ratan Sircar Medical College & Hospital, Kolkata for a duration of seven months (June 2020 to December 2020). 8,455 samples were found to be inconclusive (Table 1).
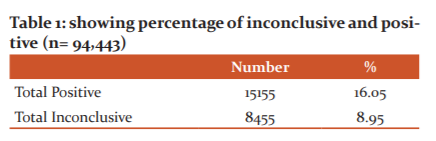
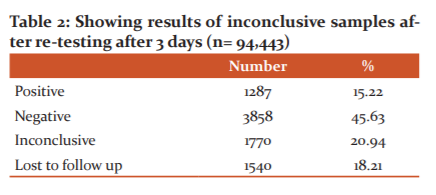
All inconclusive samples were subjected to re-testing (from repeat samples) after 3 days. Out of which, 1287 (15.22%) became positive and 3858 (45.63%) became negative [Table 2]. 1770 (20.94%) samples were found to be inconclusive again. In 1540 (18.21%) cases, they didn’t send their samples again to our Laboratory for re-testing (lost to follow up).
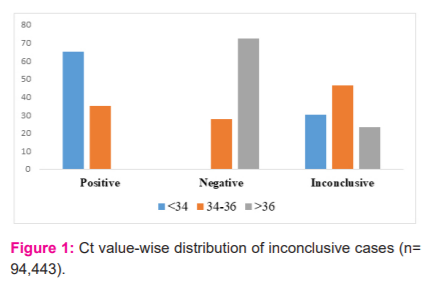
Ct value of these inconclusive results was analyzed and found that among positive samples, 64.96% had Ct value <34, whereas, among negative samples, 72.37% had Ct value >36 [Figure 1].
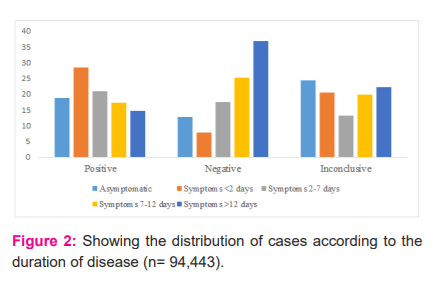
When all the cases were distributed according to the duration of disease, among positive cases, maximum patients (28.36%) had symptoms of less than 2 days’ duration, whereas, among negative cases, 36.86% cases had symptoms of more than 12 days’ duration (Figure 2).
Discussion
During COVID 19 pandemic in India, there had been a spurt in ‘inconclusive’ reports that are leaving patients and clinicians baffled and postponing treatment. There may be various reasons for being only “one target gene” positive starting from sampling error to a technical error in consideration of the dynamics of target genes like N and ORF1ab gene.
We found that 8.95% of COVID RT PCR reports became ‘inconclusive’ in our study. Although It has been noted that up to 5% of COVID RT-PCR reports may be inconclusive [8]. It may be due to low viral load, faulty sample collection and transport and technical issues related to RNA extraction.8 When all inconclusive samples were subjected to re-collection, RNA extraction and re-testing by RT PCR after 3 days, 15.22% cases became positive whereas 45.63% cases turned negative. When these inconclusive reports were analyzed according to Ct value, 64.96% positive cases after retesting had Ct value <34 whereas, 72.37% negative cases had Ct value >36. Again, after comparing these cases with the duration of disease, it was found that among positive cases, maximum patients (28.36%) had symptoms of less than 2 days’ duration, whereas, 36.86% cases had symptoms of more than 12 days’ duration among negative cases.
This can be explained in this way that during the pre-symptomatic phase of infection, when the virus started to replicate and the disease curve started to ascend, the viral load is too low to detect or may detect one target gene, which when tested later after 3 days turned to be positive. Being asymptomatic or pre-symptomatic cases of less than 2 days’ duration, most of the inconclusive reports with Ct value <34, became positive on re-testing. Thus, a lower Ct value (<34 of one detected target gene) in inconclusive results increases the probability of being positive while re-testing after 3 days. This theory may also be implied for the negative results. At the later stage of disease, especially after 10-14 days, when the disease curve is about to touch baseline, one target gene may be detected again due to low viral load or presence of remnants of RNA or degraded RNA which when tested after 3 days become negative. Higher Ct value (>36) here indicating the increased probability of being negative on re-testing.
Out of total inconclusive samples, 1770 (20.94%) samples became inconclusive again after re-testing. When these cases were analyzed according to the duration of disease, most of the patients (24.41%) were asymptomatic or found of having symptoms of <2 days (20.56%), followed by 22.20% of cases with symptoms within >12 days’ duration. Most of the cases (46.55%) having Ct value within 34-36. This may happen due to various reasons such as – (a) beta coronavirus infections which are not due to SARS-COV2, (b) different analytical sensitivity of individual viral gene PCR, especially at low viral load and (c) nonspecific binding of PCR primer or probe during the late phase of PCR cycles (e.g. after 35 cycles).8 It may be due to problems associated with RNA extraction or due to faulty sample collection, storage and transport procedure.8 It may also because descension of the curve towards baseline is delayed due to aberrant or low immunological activity of patients and it persists for a long time beyond 12 days in samples at low concentration.
We lost for follow up in 1540 (18.21%) cases, as repeat samples were not sent again for further testing. Probable reasons behind it may be that these cases improved symptomatically or may be expired or samples were sent to another laboratory for re-testing due to changing testing strategy of the State Health Department.
Conclusion
An inconclusive result means the patient may be in the recovery stage or very early (pre-symptomatic) stage of infection. Inconclusive results most probably reflect low levels of virus in the sample but may also be due to sampling error, presence of remnants of RNA or degraded RNA or cross-contamination. In these cases, a second swab should be collected 3 days after the first test and re-tested. If the second test is negative, the patient will be considered as negative for COVID. If the second test is positive, the patient will be considered positive for COVID but If the second test remains inconclusive, interpretation is challenging. This patient should be evaluated with clinical symptoms and CT images and advised accordingly to continue home/hospital isolation. Ct value and duration of the disease of these cases may be a clue whether it is going to be positive or not on re-testing. It is also important that the clinician and various stakeholders (infection control experts) are explained about these possibilities. The counselling of the patient and relatives is also important. 8 Sample collection, RNA extraction or testing should always be done meticulously. Quality control and quality assurance of the whole testing procedure including the pre-and post-analytical parts are also essential.
Acknowledgement: I am sincerely giving thanks to the Head of our Institute for his support and kind cooperation. The authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors/editors/publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
Conflict of interest: Nil
Source of funding: Nil
References:
1. Doherty DT, Moran R, Kartalova-O’Doherty Y. Psychological distress, mental health problems and use of health services in Ireland. Dublin: Health Research Board. Health Res Board Res Ser 2008;5:14.
2. Kessler RC, Andrews G, Colpe LJ, Hiripi E, Mroczek DK et al. Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychol Med. 2002;32(6):959-976.
3. Koochaki GM, Charkazi A, Hasanzadeh A, Saedani M, Qorbani M et al. Prevalence of stress among Iranian medical students: a questionnaire survey. East Mediterr Health J. 2011;17(7):593-598.
4. Lyons Z, Wilcox H, Leung L, Dearsley O. COVID-19 and the mental well-being of Australian medical students: impact, concerns and coping strategies used. Aus Psychiatry. 2020;28(6):649-652.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License