IJCRR - 6(19), October, 2014
Pages: 34-37
Date of Publication: 10-Oct-2014
Print Article
Download XML Download PDF
EFFECT OF THYROID HORMONES IN MALES WITH INFERTILITY - A CROSS SECTIONAL STUDY
Author: G. Rekha, V. Rajitha, K. Y. Manjunath
Category: Healthcare
Abstract:Background: Various authors have studied the effect of thyroid hormones to estimate the male factor in infertility. Some have concluded that thyroid hormones have a role to play in determining the quality of sperms and some state that the hormones do not have any effect on spermatogenesis. This study was done to observe the effect of thyroid hormones in the affected males. Materials and Methods: The male partners of 71 infertile couples participated in the study. Semen analysis was done in the affected males after an abstinence of three days. Thyroid hormones estimation and semen analysis was done on the same day. The males were grouped as Oligospermic, severe Oligospermic and Azoospermic after semen analysis. Normospermic males were used as a control group. Result: The age range of the affected males was 24 \? 53 years. The mean years of marital duration were 7.7 years. The thyroid hormonal level was within normal limits in all the 71 males investigated. In semen analysis, 17 males were Normospermic. 22 males were Oligospermic, 22 were severe Oligospermic and 10 were Azoospermic. The mean sperm count was 9.18 million/ ml in Oligospermic, 3.3 million/ml in severely Oligospermic, Nil in Azoospermic and 123.86 million/ml in Normospermic males. Conclusion: Thyroid hormones do not have any effect on spermatogenesis in males.
Keywords: Thyroid, Hormone, Infertility, Oligospermia, Azoospermia
Full Text:
INTRODUCTION
Infertility affects a significant number of married couples and the desire to beget a child in the affected population is of utmost importance in their lives. Out of every affected 100 affected couples, the male and the female factors are almost on par and the latter being marginally higher1 . In some cases, the cause is unknown and infertility can also occur with both the partners being affected. For investigation of the male factor in the affected couples, semen analysis is of prime importance. The quality and quantity of semen determines a positive conception when the affected factor is male. In a significant percentage the affected partner in infertility is usually a male2 . In affected male partners of infertile couples, the quality and quantity of semen differs. A recognizable decline in the semen quality been also observed in the south Indian population3 . Sex hormones play an important role in spermatogenesis which maintains the sperm quality and quantity. Many studies have elaborated the influence and importance of sex hormones in spermatogenesis and sperm count. Thyroid hormones play a significant role in the metabolism of the human body and also in the reproductive cycle in females. However not many studies exist which elucidate the effect of thyroid hormones in spermatogenesis. Many studies highlight the effect of thyroid hormone in female reproduction hence this study aims to probe the influence of thyroid hormones in spermatogenesis, sperm quality and quantity in affected males. In many studies on animal models like rats and goats demonstrate the presence of thyroid receptors in the testis especially in the sertoli cells. This regulation of thyroid hormone in animal models has been brought upon by the hypothalamo hypophyseal testicular axis which governs the sperm production. In humans the presence of thyroid receptors in the sertoli cells are disputed. In specific T3 does not inhibit receptors in the testis and the role of thyroid regulating hormone on the testis is indeterminate4 .
The presence of thyroid receptors in the sertoli cells in animal models influence germ cell production and maturation. The presence of Sertoli cells to the germ cells in humans is 1:11 when compared to the animal model. In humans thyroid hormones do not seem to influence spermatogenesis according to standard texts.
Materials and Methods
71 male partners of infertile couples attending the infertility clinic in a tertiary care hospital volunteered to participate in the study. After sexual abstinence of three days, the volunteers were made to collect semen in a sterile container which was analyzed using automated sperm analyzer. Prior to semen analysis, blood sample was collected in a sterile container and estimation of thyroid hormones was done.
Parameters of semen Analysis were determined based on WHO guidelines 20107 .
- Age - Marital status
- Volume of semen
- Ph - Sperm concentration
- WBC concentration
- Liquefaction duration
Thyroid hormone estimation was done to find the serum levels of
- T3
- T4
- TSH
Based on the sperm count the volunteers (n=71) were classified into four groups
Group -1 = Oligospermic males (22)
Group -2 = Severe Oligospermia (22)
Group -3 = Azoospermia (10)
Group -4 = Normospermic males (Used as a control group) (17)
Statistical Analysis
The observations and the numerical quotients obtained from the study were statistically analyzed using SPSS software version 16 to ascertain the statistical significance of the study.
Results
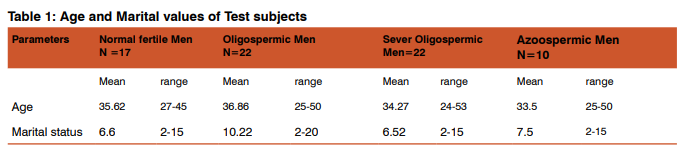
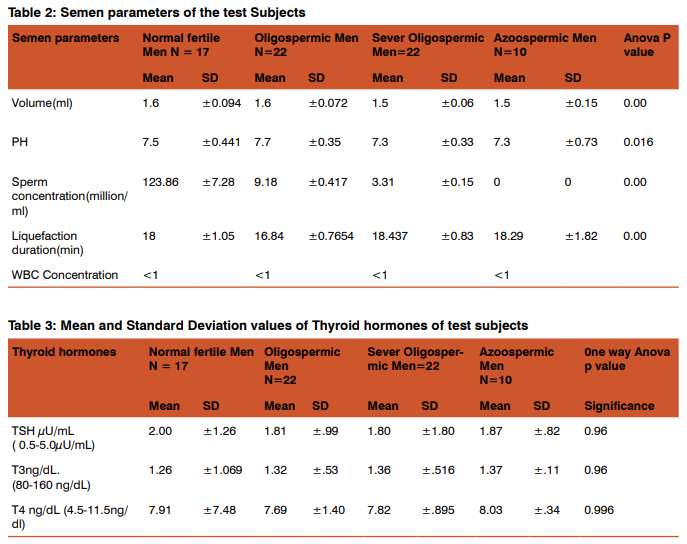
The age range of all the volunteers was from 24 - 53years with a mean of 35 years. The duration of married life in the affected couples was 2-15 years with a mean of 7.7years; Group wise distribution is depicted in Table -1. The parameters of semen analysis are depicted in Table -2. The thyroid hormone level estimation in the group wise was within normal limits in all the 71 males investigated. Group wise distribution of thyroid hormones T3, T4 and TSH estimation is depicted in Table -3. Analysis of variables for thyroid hormones is depicted in Table -3. In semen analysis, 17 males were Normospermic. 22 males were Oligospermic, 22 males were severe Oligospermic and 10 males were Azoospermic. The mean sperm count was 9.18 million/ml in Oligospermic males, 3.3 million/ ml in severely Oligospermic males, Nil in Azoospermic males and 123.86 million/ml in Normospermic males. Analysis of variables for the sperm count is depicted in Table -2.
Discussion
Thyroid hormones have effect on spermatogenesis in animal models, as receptors are present in the testis and influence the quality of sperms. Some authors have studied the effect of thyroid hormones on the quality of sperms but a direct and conclusive evidence still eludes5 . These studies elaborate the effect of sertoli cells rather than on the germ cells. Since such studies have been done on smaller sample size, the actual cause and effect in the case of thyroid hormones cannot be definitely established. However some studies have indicated that there is deterioration in the quality of sperms due to defective spermatogenesis arising primarily out of morphological abnormalities of sertoli cells6 . Few authors have suggested that hormonal therapy should be considered for treating hormonal insufficiency and a reproductive endocrinologist should be included to perform a hormonal assessment which should be made a part of investigations for male infertility8 . Semen analysis is the sole and reliable test to estimate the male factor in infertility. Since a majority of male factor in infertility is due to deficient sperm count and abnormal sperm parameters which is due to a error in the control mechanism of pre and post testicular reasons9 . LH and FSH have more significant role to play in spermatogenesis as they stimulate gametogenesis than thyroid hormones. Although other endocrine hormone receptors are found in the parts of the male reproductive system, it is highly unlikely that hormones other than LH and FSH influence the outcome of spermatogenesis in cases of male infertility10. Studies performed in males with infertility to find out the relationship between hypothyroidism and spermatogenesis have also primarily state that the effect of FSH and LH on the testis and sertoli cells in particular conclude that the influence of the above mentioned hormones are not direct11. Most of the studies which establish a link between hypothyroidism, hyperthyroidism and spermatogenesis have been performed in western subjects and not many studies exist on Indian test subjects and the one such study done does not find any significant effect of thyroid hormones in male infertility12.
Conclusion
To conclude this study does not establish any direct link between thyroid hormones and spermatogenesis in male infertility. However since the sample size of this study is relatively modest, extending the study with a larger sample size might validate the present findings. Also widening the parameters and methodology with repeated blood samples and semen analysis might establish a direct effect on thyroid hormones on spermatogenesis in males with infertility.
ACKNOWLEDGEMENTS
The authors sincerely wish to thank the management, administrators and the Professors and Head of the department of Anatomy of Vinayaka Missions Kirupananda Variyar Medical College, Salem for their whole hearted support and permissions to utilize their resources and conduct this study. The authors acknowledge the great help received from the scholars whose articles cited and included in references of this manuscript. The authors are also grateful to authors/editors/publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed. Authors are grateful to IJCRR editorial board Members and IJCRR team of reviewers who have helped to bring quality to this manuscript.
References:
1. K Poppe, D Glinoer, H Tournaye, Is systematic screening for thyroid disorders indicated in sub fertile men? European Journal of Endocrinology 2006:154 363–366.
2. S.Bhasin, D.M.DE Kretser, H.W.G.Baker , Clinical Review 64 Path physiology and natural History of Male Infertility. Journal of clinical Endocrinology and metabolism; vol.79, No.6.
3. Adiga SK, Jayaraman V, Kalthur G, Upadhya D, Kumar P. Declining Semen quality among South Indian infertile men : A retrospective study. J Hum Reprod Sci Issue 1 Jan –Jun 2008.15-18
4. Francis. S. Greenspan, Gordon J. Strewler Control of Thyroid function, Basic and Clinical Endocrinology, 5th Edition, 207- 217.
5. Rajender singh, Alaa J Hamada and Agarwal. Thyroid Hormones in Male Reproduction and Fertility; Central Drug Research Institute; Lucknow. The open Reproductive Science Journal, 2011:3; 98-104.
6. Sharpe RM. Declining sperm counts in men: is there an endocrine cause? J Endocrinol 1993; 136:357-60.
7. World Health Organization 2010 .WHO laboratory manual for the examination and processing of human semen - 5th edition, pg-225.
8. M.A.Emokpae,P.O Uadia,A.Z.Mohammed and A. Omale-Itodo. Hormonal abnormalities in Azoospermic men in kano, northern Nigeria. Indian J Med Res 124, September 2006, 299-304.
9. Teruaki I wamoto, Shiari Nozawa and Miki Yoshiike. Semen quality of Asian men; Reprod Med Biol 2007; 6:185- 93.
10. Muhammad Shoaib Khan, Irshad Ali et al: Determination of Serum Gonadotropin and Testosterone Levels in Male Infertility. JPMI 2007 Vol.21No.02:86-91.
11. Elzbieta Krajewaka –Kulak and Pallav Sengupta. Thyroid function in male infertility. Frontiers in Endocrinology. November 2013, Volume 4, Article 174/1.
12. Manoj Kumar Sharma, Deepak Parchwani et al; Relationship between thyroid profile and Semen Quality, National Journal of Community Medicine Vol 3 Issue 1 Jan –March 2012:20-24.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License