IJCRR - 8(19), October, 2016
Pages: 12-16
Print Article
Download XML Download PDF
IN-VITRO SUSCEPTIBILITY TO TIGECYCLINE IN MULTIDRUG RESISTANT BACTERIAL ISOLATES FROM A TERTIARY CARE HOSPITAL
Author: Kusuma G.R., Tejashree A., Vijay Kumar G.S.
Category: Healthcare
Abstract:Objective: The present study was conducted to evaluate the in vitro activity of tigecycline against a contemporary collection of multidrug resistant (MDR) bacterial isolates by disc diffusion and MIC by E-Test method.
Methods: A total of 100 non repetitive clinically significant MDR bacterial isolates from urine, pus, sputum endotracheal aspirates, Skin and soft tissue and surgical site infection of patients in a tertiary care teaching hospital in Karnataka, south India from March 2013 to December 2013 were included in the study. MDR bacteria tested for Tigecycline susceptibility were: Methicillin resistant S.aureus (MRSA) (15), ESBL producing Escherichia coli (E.col) (15), Klebsiella pneumoniae (35) and MDR Acinetobacter species (35).
Result: Tigecycline was found to be effective against all MRSA, MDR E.coli and Acinetobacter isolates by disc diffusion and E-test method. Among the selected K. pneumoniae isolates all were sensitive by disc diffusion and 34 (97.1%) were found sensitive with the MIC range 0.25- 1.5\?g/ml, One (2.9%) isolate was found intermediate resistant with the MIC of 3\?g/ml by E-test.
Conclusion: To conclude, the present study showed that, tigecycline is a potent antimicrobial agent against MRSA, ESBL producing Enterobacteriaceae Acinetobacter species and disc diffusion is simple to perform, highly reproducible and inexpensive method to predict tigecycline resistance. It is also prudent to reserve tigecycline for life threatening infections.
Keywords: Tigecycline, MDR, E-Test, India
Full Text:
INTRODUCTION
Antimicrobial resistance has been identified as one of the major challenges facing public health, as it has increased rates of morbidity, mortality and socioeconomic costs1.
The rates of multiple drug resistance are increasing among Enterobacteriaceae, metallo beta lactamase [MBL] producing non fermenting gram negative bacilli and Gram-positive pathogens such as methicillin resistant Staphylococcus aureus [MRSA] vancomycin resistant enterococci [VRE] that commonly cause serious life-threatening diseases and present a challenge for clinicians by limiting the potentially active antimicrobial agents to treat. Thus, the development and evaluation of new antimicrobial agents that overcome existing mechanisms of resistance is urgently needed.2
In this scenario, research has led to development of a new group of drugs called glycylcyclines, a broad spectrum tetracycline analogues that overcome the resistance mechanisms and the most promising compound being the tigecycline, a glycyclamido derivative of minocycline3
Tigecycline [TGC] is the first of a new class of modified tetracycline antimicrobials known as glycylcyclines. It exerts its bacterostatic effect by binding to the bacterial 30S ribosome and inhibits protein biosynthesis, but its unique feature is its ability to evade the major determinants of tetracycline resistance, that provide ribosomal protection. Its structural modification is the addition of a 9-t-butyl-glycylamido side chain to the central skeleton of minocycline . This provides the drug with an expanded spectrum of activities, including those against susceptible and multidrug-resistant Gram-positive and Gram-negative organisms, anaerobes, and atypical Mycobacteria but tigecycline has poor activities against certain organisms, most importantly Pseudomonas spp. and Proteus spp. as they carry inherently encoded resistance-nodulation-division (RND) efflux pumps that confer decreased sensitivity.4&5
Tigecycline was approved in 2005 by the U.S. Food and Drug Administration (FDA) and in 2006 by the European Medicines Agency for the treatment of complicated skin and skin structure infections and complicated intra abdominal infections 6
Thus the present study was conducted to evaluate the in vitro activity of tigecycline against a contemporary collection of multidrug resistant bacteria isolated from clinical specimens, by disc diffusion and MIC by E-Test method.
Materials and Methods:
This prospective study was conducted in the microbiology department, at JSS Hospital, Mysore a Tertiary Care Teaching Hospital in Karnataka, South India from March 2013 to December 2013.
A total of 100 non repetitive clinically significant MDR bacterial isolates were included in the study. Susceptible bacteria, Pseudomonas spp. and Proteae were excluded from the study as tigecycline has decreased activity against Pseudomonas and Proteae.
The specimens such as urine, pus, sputum and endotracheal aspirates ,swabs from skin and soft tissue and surgical site infection received for culture and sensitivity testing from various departments in our hospital were immediately processed and initial isolation , identification and antibiotic susceptibility testing was done according to standard recommended procedure in the clinical laboratory.7
All Gram negative pathogens were tested for extended spectrum beta lactamase [ESB production by CLSI phenotypic confirmatory method using ceftazidime (CAZ) and ceftazidime +clavulinic acid (CAZ+clav) disc according to CLSI guidelines Acinetobacter species were tested for MBL production by imipenem-EDTA combined disk test11. Screening of MRSA was done by using cefoxitin (30μg) disc. Interpretation was done according to clinical laboratory standards institute [CLSI] guidelines8.
MDR Gram negative bacterial isolates and MRSA randomly selected for tigecycline susceptibility testing by disc diffusion & E –test were MRSA (15), ESBL producing Escherichia coli [E.coli] (15), Klebsiella pneumonia (35) and MDR Acinetobacter species (35), both MBL and non MBL producers were included.
Selected isolates were tested for tigecycline susceptibility by Kirby Bauer disc diffusion method using commercially available tigecycline (15μg) disc. [Hi media]. S.aureus strain 25923 and ATCC E.coli strain 25922 were used as control.7&8.
The minimum inhibitory concentration of tigecycline for all the selected MDR bacteria was done by E- Test method .The E-test strips were procured from Biomeriux SA, France, and the test was performed according to manufacturer’s instructions. Since there were no CLSI recommended interpretative criteria for MIC of tigecycline, the US FDA breakpoints were used.For Enterobacteriaceae sensitive isolates were those with MIC ≤ 2μg/ml, and ≥ 19 mm zone size and resistance was defined as MIC ≥ 8 μg/ml and zone size ≤ 14 mm. For S. aureus MIC ≤ 0.5μg/ml and ≥ 19mm zone size was considered sensitive 9
RESULTS
All randomly selected MRSA [15] isolates for tigecycline susceptibility testing by disc diffusion & E –test were found susceptible to tigecycline by both methods. The MIC range by E-test was 0.125 – 0.032μg/ml .The range of diameter of the zone of inhibition around tigecycline disc was 19mm -25mm.There was a gradual reduction of tigecycline zone diameter as the MICs for the isolates increased.
All selected E.coli [15] and K.pneumoniae [35] isolates were ESBL producers and resistant to Amikacin , Gentamycin, Cephalosporins, Ciprofloxacin, Cotrimoxozole. Among K.pneumoniae isolates 30 were resistant to Piperacillin/tazobactam and 06 isolates were resistant to Imipenem.
Susceptibility to tigecycline among E.coli isolates was found 100% by both methods. MIC range by E-test was 0.064 – 0.25μg/ml. The diameter of the zone of inhibition around tigecycline disc was in the range of 21mm – 25mm and there was correlation between MIC and disc diffusion.
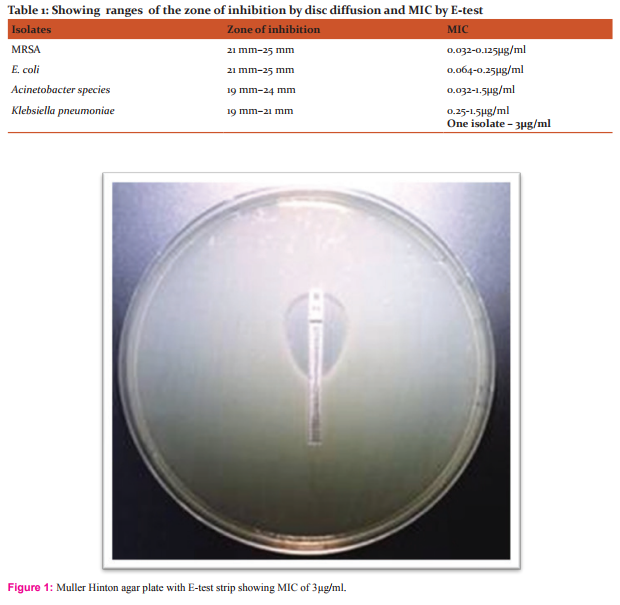
Among the selected K.pneumoniae isolates, 34(97.1%) were found sensitive by E-test with the MIC range 0.25- 1.5μg/ml. One isolate was found intermediate resistant with the MIC of 3μg/ml. All isolates were in the sensitive range 19mm – 21mm by disc diffusion .
Acinetobacter species [35] were resistant to Amikacin, Gentamycin, Tobramycin, Cefipime, Piperacillin/ tazobactam and Ciprofloxacin .11 isolates were resistant to Imipenem.
By disc diffusion method all Acinetobacter species were in the sensitive range. The zone of inhibition remains between 19mm-24mm. All isolates were found to be sensitive with the MIC range between 1.5 – 0.032 μg/ml by E-test.
Discussion
Tigecycline shows high potency against Gram-negative bacilli belonging to family Enterobacteriaceae in whom multi-drug resistant strains have emerged as important nosocomial pathogens. Tigecycline is also very active against non-fermentative GNB, such as Acinetobacter species. and tigecycline has promising microbiological, pharmacodynamics & pharmacokinetic profile .Therefore it is considered as a good alternative to treat infections due to multidrug resistant organisms.10
In our study tigecycline showed 100% activity against all, MRSA by a concentration of ≤0.25 μg/ml of tigecycline with a zone of inhibition of ≥ 19mm. The results of our study were in concordance with study conducted by Bijayani Behra et al11, Rouchelle Tellis et al6, Manisha Mane et al13, Maria Souli et al12
ESBLs are one of the most evolving mechanism of antibiotic resistance among the family Enterobacteriaceae and therapeutic options are limited. Although Carbapenems are the drug of choice in the treatment of infections due to ESBL producing strains of Enterobacteriaceae, the emergence and proliferation of bacteria resistant to this important group of drug is jeopardizing the use of carbapenems and options are limited to tigecycline, colistin and polymyxin 13&14 .
In our study tigecycline remains an important option against the management of E.coli infections by retaining 100% in vitro activity against E.coli isolates with the MIC90≤0.25. µg/ml by E-test. All isolates showed zone of inhibition ≥ 19mm. the zone diameter remains within a range of 21mm- 25mm.and shows the correlation between E-test and disc diffusion. Similar results were found in studies conducted by Soham Gupta et al, Shanti. M et al15 , Anand Manoharan et al16, Rouchelle Tellis et al, Te-Din Huang et al17 ,Goran Kronvall et al18 .
Among our selected K. pneumoniae isolates 34/35 (97.1%) were found sensitive with the MIC range 0.25- 1.5μg/ml. One isolate was found intermediate with the MIC of 3μg/ml by E-test. None were found resistant /intermediate by disc diffusion. All the isolates showed zone of inhibition ≥ 19mm. the zone diameter remains within a narrow range of 19mm- 21mm.Other studies by Shanthi.M et al 100%, Anand Manoharan et al,100% Simit Kumar et al19 100% Bijayini Behera et al 97% Soham Gupta et al20 85.7% also showed high in vitro activity of tigecycline against K.pneumoniae. In the study conducted by Subhash C. Arya2166% were found sensitive. It was also noted that in our study, increased MIC of 1-3µg/ml in K.pneumoniae compared to E.coli with MIC90≤ 0.25µg/ml. Similar results with increased MIC were found by Soham Gupta et al, and Maria Souli et al.
Break points for Tigecycline MIC and disc diffusion for Acinetobacter were not included in the CLSI guidelines. Therefore cut off values given for Enterobacteriaceae were used and all selected Acinetobacter species isolates were in the sensitive range. The zone of inhibition between 19 mm-24 mm. The MIC remains between 0.75 – 0.032 μg/ml with MIC90 ≤0.75 by E-test. It was observed that there was gradual reduction in the size of zone of inhibition as MIC increases .This was also observed by Bijayini Behera et al In our study, the E test correlated 100 percent with the inhibition zone diameters, which was in contrast to the findings of a study which was done by Behera et al. But, it was similar to the findings of a study which was done by Venezia et al22,Surapee Tiengrim A et al23.
In our study Tigecycline remains as a good option for the management of MRSA, multidrug resistant E.coli , Klebsiella species and Acinetobacter infections by retaining 100% activity against these pathogens
We carried out the in-vitro activity of tigecycline by disc diffusion and E test. By both methods all isolates were found to be sensitive except one Klebsiella isolate which was found to be intermediate by E-test and sensitive by disc diffusion. Thus we found no significant difference between these two methods. Disc diffusion method is simple to perform, highly reproducible and inexpensive while E test is though costly for routine use, it can be used to determine MIC.
Tigecycline does not require dose adjustment in patients with impaired renal function and is conveniently administered every 12 h. It has a long terminal half-life and a large volume of distribution and has low potential for organ toxicity and drug-drug interactions. These properties make the use of this antibiotic relatively uncomplicated, but patients may develop moderate-to-severe nausea and vomiting during tigecycline therapy. It can be used as a life saving antimicrobial in polymicrobial infections due to Gram-positive and enteric Gram-negative bacteria.
Conclusion
The present study shows that, tigecycline is a potent antimicrobial agent against MRSA, ESBL producing Enterobacteriaceae and multi-drug resistant Acinetobacter baumannii and disc diffusion is simple to perform, highly reproducible and inexpensive method to predict tigecycline resistance. However, use of tigecycline needs to be strictly monitored to prevent development and dissemination of resistance against this one of the last available antimicrobial molecule and it is prudent to reserve tigecycline for life threatening infections.
Acknowledgement
Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors / editors / publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
References:
- Cai Y, Wang R, Liang B, Nan B, and Liu Y. Systematic Review and Meta-Analysis of the Effectiveness and Safety of Tigecycline for Treatment of Infectious Disease. Antimicrobial agents and chemotherapy 2011: 1162–1172.
- Kelesidis T, Drosos E. poulos K, Kelesidis. I and Matthew E. Tigecycline for the treatment of multidrug-resistant Enterobacteriaceae: a systematic review of the evidence from microbilogical and clinical studies. Journal of Antimicrobial Chemotherapy (2008); 62 :895–904.
- Gupta K, Kaushal S, Chopra S. C. Tigecycline: A novel glycil cycline antibiotic. Indian J Pharmacol 2006 June , 38 ; Issue 3 : 218-19
- Rossi F, Andreazzi D .Overview of Tigecycline and Its Role in the Era of Antibiotic Resistance The Brazilian Journal of Infectious Diseases 2006; 10(3):203-216.
- Anton YP, Adams J,. Paterson DL. Tigecycline Efflux as a Mechanism for Non susceptibility in Acinetobacter baumannii._Antimicrobial Agents And Chemotherapy, June 2007: 2065–2069
- Tellis R, Rao S, Lobo A Dept. of Microbiology, An in-vitro study of tigecycline susceptibility among multidrug resistant bacteria in a tertiary care hospital . International Journal of Biomedical Research IJBR 2012 March; 3 [04]: 192?195
- Winn C, Allen D, Janda M, Koneman WE, Procap W. Schreckenberger C, Woods L Koneman’s color atlas and text book of diagnostic Microbiology. The role of the Microbiology Laboratory in the diagnosis of infectious diseases: Guidelines to practice and management.6th edition New York :Lippncott Williams and Wilkins:2006.p 2-61
- Clinical and Laboratory Standards Institute. Performance standards for antimicrobial susceptibility testing: CLSI document M100-S22. Wayne, PA: Clinical and Laboratory Standards Institute, 2012
- Wyeth Pharmaceuticals. Tygacil (tigecycline) for injection [Package insert]. 2005. Wyeth Pharmaceuticals Inc., Philadelphia, PA. NDA 21-821/S-016
- Daryl J, HobanaT, Bouchillona SK, Brian M, Jack J, Johnsona L, Michael JD .In vitro activity of tigecycline against 6792 Gram-negative and Gram-positive clinical isolates from the global Tigecycline Evaluation and Surveillance Trial (TEST Program, 2004) Diagnostic Microbiology and Infectious Disease ;52 (2005): 215–227
- Behera B, Das A, Mathur P, Kapil A, Gadepalli R , Dhawan D. Tigecycline susceptibility report from an Indian tertiary care hospital. Indian J Med Res 129, April 2009: 446-450
- Souli M ,Flora V, Koratzanis K E, Antoniadou A, GiannitsiotiE, Evangelopoulou P, Kannavaki S and Giamarellou H. In Vitro Activity of Tigecycline against Multiple-Drug-Resistant, Including Pan-Resistant, Gram-Negative and Gram-Positive Clinical Isolates from Greek Hospitals. Antimicrobial Agents And Chemotherapy, Sept. 2006: 3166–3169
- Manisha M, Nita G. In Vitro Activity of Tigecycline against Methicillin Resistant Staphylococcus aureus (MRSA) and Vancomycin resistant Enterococci (VRE) As Evaluated by Disc diffusion method and E-test .International Journal of Collaborative Research on Internal Medicine & Public Health (2013);Vol. 5 No. 8: 567
- Priya D, Varsha G, Shivani G, Jagdish C, Phenotypic method for differentiation of carbapenemases in Enterobacteriaceae: Study from north India ,Indian jornal of Pathology and Microbiology july - september 2012; 55(3 ) ;357-60
- Shanthi M, Uma S. Invitro Activity of Tigecycline Against GramPositive and Gram Negative Isolates in a Tertiary Care Hospital . Journal of Clinical and Diagnostic Research.2011 December ;5(8):1559-1563
- Anand M, Saradiya C, S.Madan, Dilip M. Evaluation of the tigecycline activity in clinical isolates among Indian medical centre. Indian journal of Pathology and Microbiology. 53(4),Oct-Dec-2010
- Yen-Hsu C, Po-Liang L Cheng H H. Trends in the Susceptibility of Clinically Important Resistant Bacteria to Tigecycline: Results from the Tigecycline In Vitro Surveillance in Taiwan Study, 2006 to 2010Antimicrobial Agents and Chemotherapy : 1452–1457.
- Goran K, Inga K, Mats W, Mikael S. Epidemiological MIC cut-off values for tigecycline calculated from Etest MIC values using normalized resistance interpretation. Journal of Antimicrobial Chemotherapy (2006) 57, 498–505
- Simit K, Maitreyi B, Soma M, Nupur P, Tapashi G, Manas B, Parthajit B. Tigecycline activity against metallo?beta?lactamase producing bacteria. Avicenna Journal of Medicine / Oct-Dec 2013; 3 Issue 4
- Soham G, Aruna C, Savitha N, Mary D and Muralidharan S. In vitro activity of tigecycline against multidrug-resistant Gram-negative blood culture isolates from critically ill patients. J Antimicrob Chemother 2012
- Subhash C.A, Nirmala A .Tigecycline in-vitro susceptibility and antibiotics fitness for gram negative pathogens. MED J.2008;vol.29(11);1558-1560
- Navon-Venezia S, Azita L, and Yehuda C. High tigecycline resistance in multidrug-resistantAcinetobacter baumannii . Journal of Antimicrobial Chemotherapy 2007 ;59: 772–774
- Surapee T, Chanwit T, Visanu T.In Vitro Activity of Tigecycline against Clinical Isolates of Multidrug-Resistant Acinetobacter baumannii in Siriraj Hospital, Thailand.J Med Assoc Thai 2006; 89 (Suppl 5): S102-5
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License