IJCRR - 10(4), February, 2018
Pages: 25-28
Date of Publication: 17-Feb-2018
Print Article
Download XML Download PDF
Correlation of High Sensitivity C-Reactive Protein and Carotid Intimal Medial Thickness in Patients with Ischemic Stroke
Author: Virendra Atam, Arpit Gupta, Sciddarth Koonwar, Manoj Kumar, Isha Atam
Category: Healthcare
Abstract:Background: Stroke is defined as an acute neurological deficit lasting more than 24 hours and caused by cerebrovascular etiology. It is further subdivided into ischemic stroke (caused by vascular occlusion or stenosis) and hemorrhagic stroke (caused by vascular rupture, resulting in intra parenchymal and/or subarachnoid hemorrhage).
Aim: Our study was designed to study the levels of High sensitivity C reactive protein (HsCRP), which is a marker for chronic inflammation, in patients with ischemic stroke due to large vessel atherosclerosis and correlate it with carotid intimal medial thickness.
Methodology: This study was done in Department of Medicine and Department of neurology in KGMU, Lucknow, between August 2016 to July 2017, and 100 patients with ischemic stroke presenting within 72 hours of onset, who met the inclusion and exclusion criteria. HsCRP was evaluated and CIMT was subsequently measured.
Result: HsCRP is significantly increased in patients with ischemic stroke. The carotid intimal medial thickness which is a proven marker for large artery atherosclerosis is also increased in patients with ischemic stroke and it is also significantly correlated with the levels of HsCRP. The levels of HsCRP is elevated more in patients with Diabetes Mellitus and Hypertension.
Conclusion: HsCRP levels are increased in patients of ischemic stroke suggesting that it could be used as a marker for the prediction of the ischemic stroke when combined with CIMT, together these two could predict the ischemic stroke.
Keywords: High sensitivity C reactive protein, Subarachnoid hemorrhage, Carotid artery, Ischemic stroke
DOI: 10.7324/IJCRR.2018.1045
Full Text:
INTRODUCTION
Stroke is defined as an acute neurological deficit lasting more than 24 hours and caused by cerebrovascular etiology. It is further subdivided into ischemic stroke (caused by vascular occlusion or stenosis) and hemorrhagic stroke (caused by vascular rupture, resulting in intra parenchymal and/or subarachnoid hemorrhage).[1]
Progressive atheromatous plaque in the carotid artery usually at the bifurcation results in gradual narrowing of the carotid artery. This process can be symptomatic but may lead to ischemic stroke or transient ischemic attack from embolization, thrombosis, orhemodynamic compromise. To measure the extent of atherosclerotic disease we measure Carotid Intimal medial thickness, which is a proven marker for the atherosclerotic large vessel disease.
High sensitivity C reactive protein is a marker of inflammation has gained importance in the recent times as a pro-inflammatory marker. Various studies have shown that HsCRP could be used as an early marker of atherosclerosis. [2]
MATERIALS AND METHODS
Our study was designed to study the levels of High sensitivity C reactive protein (HsCRP), in patients with ischemic stroke due to large vessel atherosclerosis and correlate it with carotid intimal medial thickness. This study was done in Department of Medicine and Department of neurology in KGMU, Lucknow. This study was conducted in between August 2016 to July 2017, and 100 patients with ischemic stroke presenting within 72 hours of onset, who met the inclusion and exclusion criteria.
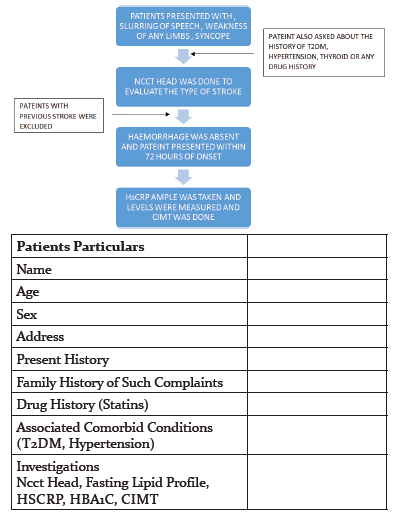
A standardized questionnaire was given that includes Name, Age, Sex or any family h/o diabetes or hypertension. Any concurrent history of hypertension, thyroid, or Diabetes mellitus was asked. All participants were asked to give informed written consent after explaining the study. The study was approved by the Ethical committee, KGMU, Lucknow. After making the diagnosis of ischemic stroke the patients were subjected to blood investigations for which approximately 5 ml venous blood sample was drawn and HsCRP levels were analyzed in those samples along with complete blood picture, S. Urea, S creatinine. Along with that if the patient wasn’t in the fasting state, then sample for fasting lipid profile was also drawn after 8 hours of fasting.
RESULTS
Statistical analysis was done by the mean, median, standard deviation and Student t-test and the significance was analyzed by the "p-value".
The mean age of the study population was 60.98±7.35. The Male-female ratio was 2.81.




The mean values of HsCRP and CIMT were increased in patients with ischemic stroke and are significantly correlated with each other. The factors which are not significant are Hb and HDL.
DISCUSSION
HsCRP which is a marker of chronic inflammation is significantly increased in patients with ischemic stroke. The carotid intimal medial thickness which is a proven marker for large artery atherosclerosis is also increased in patients with ischemic stroke and it is also significantly correlated with the levels of HsCRP. The levels of HsCRP is elevated more in patients with Diabetes Mellitus and Hypertension. As compared to the levels in patients without hypertension or diabetes mellitus, the patients having both or either one of them has increased levels. Moreover, the patients having uncontrolled Diabetes Mellitus i.e. HbA1C > 9.0 are having even more levels. The levels of HsCRP are not significantly correlated with HDL and Hb.
The results were in concordance with the following studies, Dibyaratna Patgiri1 et al [3] hsCRP is an acute phase reactant whose concentration rises in stroke as well as in those at risk. The rise may be identified even before the appearance of risk factors. Hence, hsCRP may be useful as a predictive and diagnostic marker in stroke. Liu et al [4]. We found that higher hs-CRP concentrations were associated with a higher risk of IS, particularly for non-fatal stroke, male and hypertensive subjects. In contrast, we did not observe significant associations between hs-CRP and ICH/ SAH
CONCLUSION
HsCRP levels are increased in patientswith ischemic stroke suggesting that it could be used as a marker for the prediction of the ischemic stroke when combined with CIMT, together these two could predict the ischemic stroke. As we had a small sample size, more studies need to be done to predict the role of HsCRP as a marker of ischemic stroke.
ACKNOWLEDGEMENT
Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors/ editors / publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
SOURCE OF FUNDING: NIL
CONFLICT OF INTEREST: NIL
References:
- Amarenco P, Lavallée PC, Labreuche J, et al. One-year risk of stroke after transient ischemic attack or minor stroke. N Engl J Med. 2016;374:1533-1542
- Adams HP Jr, Bendixen BH, Kappelle LJ, et al. Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke. 1993;24:35-41.
- Patgiri D. Serum hsCRP: A Novel Marker for Prediction of Cerebrovascular Accidents (Stroke). JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH. 2014
- Liu Y, Wang J, Zhang L, Wang C, Wu J, Zhou Y et al. Relationship between C - Reactive Protein and Stroke: A Large Prospective Community Based Study. PLoS ONE. 2014;9(9):e107017.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License