IJCRR - 9(16), August, 2017
Pages: 36-42
Print Article
Download XML Download PDF
Profiling of Body Hydration and Related Blood Parameters under Hot-Arid Conditions among Indian Population doing Graded Physical Activity
Author: Abhishek Bharadwaj, T. P. Baburaj, Amir Chand Bajaj, Gulab Singh, Usha Panjwani, Shashi Bala Singh
Category: Healthcare
Abstract:This study highlights the effect of extreme heat stress exposure (WBGT Index 36.24\?C) on hematological variables while performing graded physical activity (sedentary, moderate and heavy). Total 30 participants were involved in the study and were randomly distributed into batches of 10 under three categories of physical activity. Volunteers performed physically strenuous work while being exposed to ambient heat stress (hot \?arid conditions). White Blood Corpuscles (WBC) count in heavy work group [506 kcal/ hr energy expenditure] showed significant increase from pre to post exposure (p < 0.01). No other group showed significant change in WBC count. Haematocrit % (Hct %) was significantly increased among heavy work group (p < 0.01) whereas Red Blood Corpuscles (RBC) count and Red Blood Cell Distribution Width (RDW) showed no significant increase. Blood viscosity showed increase among moderate work group [412kcal / hr energy expenditure] (p< 0.05) and heavy work group (p< 0.001). These alterations indicate that participants exposed to high ambient temperature while doing graded physical activity underwent considerable hypo-hydration (sweat loss upto 4% of body weight) which got reflected in hematological parameters. This depletion of body fluid got reflected on blood viscosity and WBC count at a stage when the condition was not subjectively perceived. Data may be beneficial to identify such hypo hydration status before the condition is manifested visibly or symptomatically.
Keywords: Heat Stress, Graded work, Hypo-hydration, Blood parameters
DOI: 10.7324/IJCRR.2017.9167
Full Text:
Introduction
Tropical latitudes corroborate with warm climatic conditions ranging from arid / semi-arid terrain of desert to hot humid coastal regions. Soaring ambient temperature with intense solar radiation, warm winds and sandy terrain are salient features of desert environment. Such climatic conditions challenge the natives and also people carrying out operations (physically strenuous activities) under such environment. Desert conditions are known to cause debilitating effects on humans (1) with significant reduction in performance (9).
For maintaining a homoeothermic condition, human body toils hard to sustain thermal equilibrium (17). Result of heat exposure varies from mild discomfort, declined physical / mental ability and in extreme conditions threatening physiological conditions leading to mortality. Scarcity of potable water adds to the woe leading to altered body hydration status. During heat wave significant mortality and morbidity occurs due to heat stress and dehydration (5). Dehydration is primarily attributed to inadequate water intake caused by dysfunction of the central nervous system mechanisms controlling thirst (5). Symptoms of acute dehydration vary with the degree of water deficit. It is an established fact that hypo-hydration can lead to haemo-concentration. Reduced thirst and ingestive behavior have been reported in response to hyper-osmotic stimuli, hypovolemic stimuli and dehydration (5). Sufficient body water is required to sustain thermoregulatory function, thus losses in total body water can challenge the thermoregulatory system. A total body water deficit ?2% body mass (hypohydration) is recognized as the threshold when thermoregulatory function becomes measurably altered (19, 20). Sensation of thirst with dryness of mouth is felt at approximately 3%. The threshold for impaired exercise thermoregulation is 1% dehydration, and at 4%, decrements of 20 – 30% are seen in work capacity (8). Hypohydration decreases cutaneous vasodilation and sweating during heat stress (30, 31). Hypovolemia and hyperosmolality due to thermal dehydration also suppress thermoregulatory responses of sweating and cutaneous vasodilation, resulting in increased risk of heat illness (18). It has been often observed that non-acclimatized individuals tend to consume inadequate fluid leading to hypohydration, which can quickly result in dehydration with increased risk of heat illness / injury (27). Heat acclimatization induced effective adaptations are more pronounced after fluid-regulatory strain from permissive dehydration (11). In response to such altered hydration status, body undergoes several physiological changes. Exercise performed under such condition imposes severe strain on cardio-vascular system with finite cardiac output (CO) having to cater for increased blood flow to skin for thermal regulation (19, 28). Secretion and evaporation of sweat is important for thermoregulation but without water replenishment (hypohydration) plasma volume decreases with increased plasma osmotic pressure (hyperosmotic hypovolemia). Both osmotic and / or volume stressors delay onset and / or reduce the sensitivity of sweating and blood flow responses (19). It was also observed from study by Harrison et al (14) that exercise performed in heat reduced blood volume exacerbating strain on cardiovascular system. Altered hydration status affects the homeostasis within tissues and organs resulting in loss of plasma volume (haemo-concentration). It was further observed by Patterson et al that plasma volume was not defended more vigorously following humid-heat acclimatization. Rather a greater fluid loss may well underlie the mechanisms for enhancing plasma volume recovery when heat acclimation is induced using controlled- hyperthermia (26, 27). Sufficient body water is required to sustain thermoregulatory function, thus losses in total body water can challenge the thermoregulatory system (18). This situation aggravates further with exposure to high temperature and physical work under such conditions (9). Hypohydration may occur from voluntary fluid restriction, insufficient fluid availability or thermoregulatory sweating (18).
From the aforementioned findings, it can be deduced that strenuous activity under extensive environmental stress would lead to changes in body fluids and hematological parameters, ultimately affecting physical performance of the individual. Several hypotheses exist with regard to the physiological mechanisms responsible for heamodilution or haemoconcentration during heat exposure. Plasma volume expansion has been attributed by many to an influx of protein into the vascular volume, although some researchers attribute the same to electrolyte shifts. Though mechanism of action still remains speculative, it appears hematological parameters and plasma are crucial haemodynamic changes associated with adjustments to heat exposure (29).
Present study was carried out with two intentions:
- To characterize hematological responses under high ambient temperature. These finding may be beneficial to devise strategies for identifying hypo-hydration status much before their symptomatic expression.
- To document the effects of extreme heat stress exposure (WBGT Index 36.24°C) on hematological variables, while performing incremental graded work.
Materials and Methods:
Volunteers:
Thirty [30] participants were selected randomly without bias. They were physiologically and psychologically sound having mean age of 24 (±3.8) years, height 171 (±4.5) cm, weight 63.5 (±6.6) kg and BSA of 1.73 (±0.09) m2. The volunteers were divided into three (03) groups depending on nature of work (energy expenditure) they indulged in, viz. sedentary, moderate and heavy (8). Energy expenditure was measured during physical activity of the participant using “Actical Physical Monitor” (Actical Ver. 2.02 Mini Meter Company Inc. Bend, Oregon, USA). Sedentary group had energy expenditure of less than 3.0 Mets whereas moderate and heavy work group had Mets of 5.72 and 7.02 respectively (2). Prior to experiment, all participants provided their written informed consent, indicating they understood all procedures, risks and benefits of the study and their participation was voluntary. Testing protocol was approved by the Institutional Ethical Committee (IEC).
Experimental protocol: General:
The evening before day of exposure, participants for the study were briefed about procedure of experiment and their informed written voluntary consent was obtained. Caution was taken while briefing so as not to affect the outcome of experiments. Participants were asked to report the following morning before starting their daily routine. On the morning of exposure day, basal physiological readings were noted and blood sample drawn. Pre-exposure nude body weight was recorded [ATCO Human Weighing Balance, Mumbai, India]. Heart Rate was recorded using “Pulse Oxymeter” [Pulse Oxymeter Nellcor, USA. Model No.: N-20SA], prior to and also during exposure. Participants were issued “Actical Physical Monitor” for measurement of ‘Energy Expenditure’ during the period of exposure (Actical Ver. 2.02 Mini Mitter Company Inc. Bend, Oregon, USA).
Meteorological Parameters:
Environmental variables viz. Dry Bulb (DB) Temperature; Wet Bulb (WB) Temperature [Assmann Psychrometer THEIS, Gottingen, Germany] and Globe Temperature (GT) [measured manually using a Black Globe Thermometer] were monitored during entire exposure, along with Wind Velocity [Electronic Anaemometer, ACD Machine Control Co. Mumbai].
Black Globe was left out in open where volunteers were being exposed for determining solar heat load (radiation heat). Data from DB and WB were put onto a ‘Psychometric Chart’ for determining relative humidity (RH). From recorded data “WBGT Index” was calculated. “Solar Radiation” was also considered while computing the WBGT Index (16).
Physiological Parameters:
Blood Sampling:
All participants reported to laboratory on the morning of experiment day, before starting their assigned duties. They were asked to lie down in supine position comfortably for 5 minutes before drawing blood. A tourniquet was applied lightly and for minimum duration. With individual still in supine position venous blood was drawn and stored into vaccutainers (pretreated with EDTA K3). On conclusion of assigned duties done under heat exposure, post exposure blood samples were drawn from the same participants. Precaution was taken to maintain similar position and procedure as pre exposure sampling.
Blood Parameter Measurement:
Hematological parameters as Red Blood Corpuscles (RBC) count, White Blood Corpuscles (WBC) count, Red Blood Cell Distribution Width (RDW) and Haematocrit (Hct) % were measured. Blood parameters were measured using fully automatic ‘Hematological Cell Counter’ [MS4 Hematological Cell Counter. Melet Schloesing Lab, France]. Fresh, whole blood was used for assay. Whole blood was collected in vaccutainers pretreated with EDTA K3. After homogenization of the vaccutainers over roller, 20μl blood was aspirated by the instrument and used for assay. Assay was carried out on pre and post-exposure blood samples.
Viscosity Measurement:
Viscosity of pre and post exposure blood samples was measured from fresh whole blood using Micro viscometer (Model Cap 200L. Brookfield Engineering Laboratory, Brook Field USA). Estimation was carried out using 40 μl of blood.
Hydration Status:
During exposure a diary was maintained for noting fluid intake and urine output. Intake of fluid was documented by measuring amount of fluid consumption by the individual at every instance with help of graduated tumblers (provided to the participants on the day of experiment). Similarly, urine excretion during that period was collected in graduated jerrican. This amount of fluid intake and urine output was noted during the time of exposure while doing work. Data from water consumed, urine excreted and difference between pre and post nude body weights were used to compute sweat loss and sweat rate (15), leading to estimation of actual body hydration status of participant.
Urine and Plasma Osmolality:
To establish hydration status in different working groups’ urine osmolality was measured along with plasma osmolality. Urine sample was collected during the activity period in jerricans and osmolality measured. This was correlated with serum osmolality, which was separated from whole blood sample taken from the volunteers. Urine and serum osmolality was assayed using freezing point depression osmometry.
Statistical Analysis:
Different activity groups were compared by using One-Way ANOVA followed by Students Newman Keuls (SNK) Multiple Range Test. Data were considered significant with p < 0.05.
Result:
Meteorological Parameters:
Meteorological data are essential for assessment of environmental heat load. Physical data were collected from DB, WB, GT and wind velocity to assess intensity of prevailing heat stress. WBGT (Wet Bulb Globe Temperature) Index was computed using these data evaluated to identify the environmental work / heat load on participants during exposure. The maximum ambient temperature recorded during exposure was 42.4°C (DB), Globe temperature 57.8°C and Relative Humidity 38%. WBGT computed was 36.2°C. Maximum wind velocity (Gusting) was recorded at 12.8 m/s. [Table 1]
Haematological Parameters: Pre Vs Post Exposure:
White Blood Corpuscles Count [WBC]
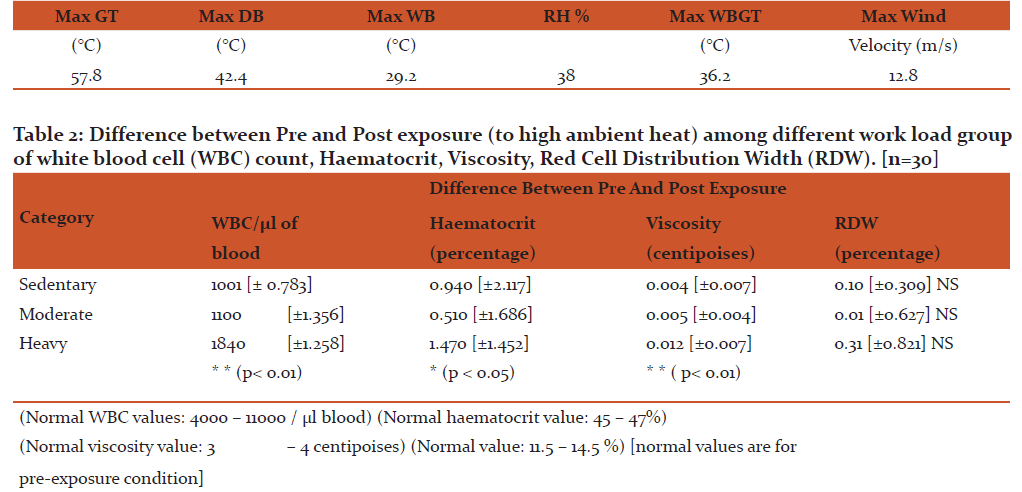
Difference was noticed in all categories of activity. Only significant difference was in ‘Heavy’ work group (p<0.01). [Table 2]
Red Blood Corpuscles Count [RBC]
Difference was evident in all the work groups but with no statistical significance.
Haematocrit Percent
There is difference seen in Hct% value between pre and post exposure among all work categories. A statistical significance is observed in heavy work category (p<0.05) [Table - 2]
Blood Viscosity
Viscosity in the pre exposure blood sample was seen to be lesser than when measured in the post exposure samples. The difference between pre and post exposure of blood viscosity is seen among every work category. A significant increase is only seen in the heavy work group. (p<0.01) [Table - 2]
Red Blood Cell Distribution Width
Red Blood Cell Distribution Width (RDW) is measure of variation of red cell volume that is reported as part of a complete blood count. Alteration in RDW is indicative of anemia in the body. RDW was measured in both pre and post exposure samples but no significant difference was observed between them, suggesting that participants were free of any anemic ailments. [Table - 2]. To corroborate the above finding and reconfirming that participants were free from any anaemic condition, mean corpuscular volume (MCV) was computed from hematocrit % and red blood corpuscular count. The general formulae used for computing MCV was:
MCV (fL) = (Hct x 10) / RBC Count.
(Refer Review of Medical Physiology, William F. Ganong, 20th edition, Mc Graw Hill Publication)
MCV signified that all participants were normal (normocytic) having values within range of 80 - 95 fL/ red cell. (values >95 fL signifies macrocytic condition and values < 80 fL signify microcytic condition)
Hydration Status:
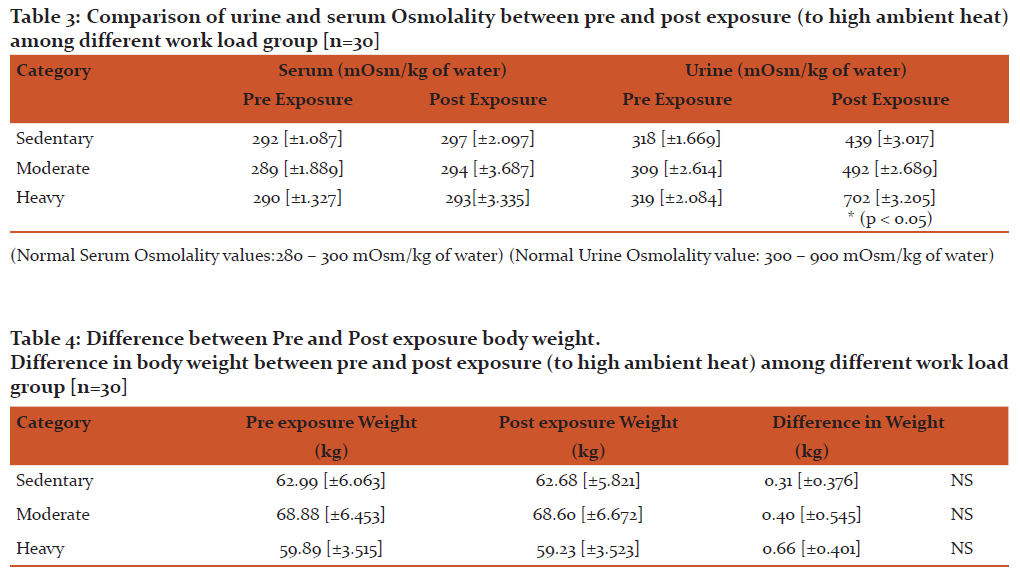
Table – 3 and 4 shows actual hydration status of participants at the end of exposure. Hypo hydration status was computed by subtracting the pre-exposure and post-exposure nude body weight. From data it is evident that volunteers in heavy work category had substantial hypohydration during exposure. Studies have established that urine osmolality is indicative of euhydration (24). In view of same along with pre and post body weight, to establish dehydration status of participant urine and serum osmolality was assayed using freezing point osmometry. Table -3 depicts the osmolality of urine and serum among the volunteers. Normal range for random urine osmolality is 300 – 900 mOsm/kg of water (23). From the results it is seen that in heavy work group the urine osmolality increased to 702mOsm/kg of water. This depicts that urine osmolaity has increased and participants under heavy work group are dehydrated. The increased osmolality corresponds to serum osmolality where in all the work groups it remained within the permissible range of 280 – 300mOsm/kg of water (7, 12, 24) depicting dehydration status of individual.
Discussion:
Maintaining homeostasis within body is prime function and requirement of life. Human body operates within very slim range of temperature. Constant interaction with external environment requires body to put in continuous effort to strike and maintain a thermal balance. People when exposed to extreme temperatures undergo several physiological changes. These physiological alterations help body adjust with hostile conditions but same time challenges the physiological limits. Body exposed to high ambient temperature gains heat thus increasing heat storage of body. This increased heat load can lead to heat related malady and even mortality. A major effect of high temperature on body is loss of body fluids. Hydration status has profound effects on both physical and mental performance (10). Both over-hydration and under hydration – if sufficiently severe- will impair performance and pose a risk to health (14, 22). Relationship between blood volume response to thermal stress and exercise cannot be understood from cardiovascular adjustments to thermal stress and exercise. Potential haemodilution and haemoconcentration depend on specific conditions, such as severity of thermal environment, intensity and type of exercise, posture, hydration and acclimatization status (3). Under exercise conditions heat – acclimatized individuals can appropriately gauge fluid intake (25, 32). Heat or exercise induced reduction in blood volume intensifies competition for available cardiac output. The magnitude of reduction in blood volume can be considerable amounting to approximately 10% of the pre-stress volume (9). This reduction exceeds the apparent decrease in blood volume that could arise from random fluctuations and measurements errors in the Hematocrit ratio and Hemoglobin concentration (13). When a change in blood volume, accompanies thermal stress or exercise, a transient shift of fluid into and out of intravascular space occurs. Once the thermal stress is removed, or exercise ceases, blood volume usually returns to the pre-stress volume (14). Greater the severity of environmental heat load, greater the tendency for haemoconcentration. Individuals may vary considerably in their intravascular volume response to thermal stress. Magnitude of exercise induced hemoconcentration is directly proportional to intensity of exercise (4).
The present study was designed to analyze effect of such high temperatures on body hydration and their reflection on hematological parameters while performing graded physical exercise. Along with body hydration status, basic hematological parameters were recorded prior to and after exposure. During exposure, individual underwent physical exertion at varied intensities. Blood parameters as White Blood Corpuscles (WBC) count, Red Blood Corpuscles (RBC) count, Haemotocrit percent (Hct %), Red Blood Cell Distribution Width (RDW) and Blood Viscosity were recorded between pre and post exposure samples, along with serum and urine osmolality (33).
The result showed significant increase post exposure [WBGT Index 36°C] mainly in the high energy expenditure group (heavy work group). WBC count among heavy work group [506kcal / hr energy expenditure] increased after exposure (p < 0.01). RBC count and RDW showed no significant increase. Blood viscosity showed significant increase among Moderate work group [412kcal / hr energy expenditure] (p<0.05) and heavy work group (p< 0.001). Hct% got significantly increased among participants working in the heavy work group under high ambient temperature. Dehydration increases hematocrit because of fluid loss, which causes a decrease in plasma volume. Due to the increased hematocrit, blood viscosity is affected showing significant increase. Previous works by Behrman and Johnson (6, 16) related dehydration with increased Hct %. Findings in the present study showed similar pattern among the Indian population, though the degree of ambient temperature exposure was remarkably higher.
Hydration data indicates hypo-hydration status of the participants but do not show any statistical significance.Hydration status of the individual got reflected in urine osmolality, though osmolality remained within physiological permissible limits but showed increased as compared to pre exposure. This depletion of fluid got significantly reflected on hematological parameters as blood viscosity, hematocrit % and WBC count.
From the findings of this study it can be concluded that heat exposure with physical exertion promotes hypo-hydration. This state gets reflected on hematological parameters of blood viscosity and WBC count at an early stage when no expression is observed in Hct%. Alterations in hematological parameter are observed at lower hypo-hydration level and much before visible symptoms are manifested in the affected individual.
Hence, it can be suggested that hematological alterations, especially blood viscosity and WBC count; may be utilized as yardstick for measure of hypo-hydration stress on healthy body before hypo-hydration condition gets expressed symptomatically.
Application: These finding can be utilized to screen individuals before exposure to extreme temperature, in order to avoid heat causalities. It can be a tool to assess hydration level of body before symptoms of hypo-hydration are manifested so as to take evasive measures before individuals complain about such occurrences.
Conclusion:
From observations of the study it can thus be concluded that changes in haematological parameters do occur, especially in blood viscosity and white blood cell count when an individual is exposed to high ambient temperature. These alterations are observed among healthy individuals even before they complain of heat related illness. These findings can be helpful in assessing hydration level of body before symptoms of hypo-hydration are manifested.
Conflict of Interest:
There is no conflict of interest.
Acknowledgement:
Authors wish to thank every individual who participated in the study and the institute for its financial support. Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors / editors / publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
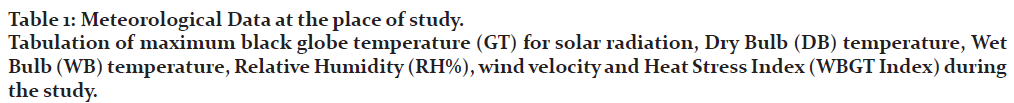
References:
- Adolph E. F, Physiology of man in the desert. New York: John Wiley and Sons, Inc. 136 -159, 1947.
- Ainsworth BE, Haskell WL, Leon AS, et al. Compendium of physical activities: classification of energy costs of human physical activities. Medicine and Science in Sports and Exercise; 25(1):71-80, 1993.
- Aukland, K., Nicolaysen, G. Interstitial fluid volume: Local regulatory mechanism. Physiol. Rev. 61: 556- 643, 1981.
- Beaumont, W. San. Underkofler, S. Beaumont, S. Van. Erythrocyte volume, plasma volume and acid- base changes in exercise and heat dehydration. J. Appl. Physiol.,
- 1255 -1262, 1981.
- Begg DP. Disturbances of thirst and fluid balance associated with aging. Physiol Behav S0031-9384 (16) 30723-5 doi: 10.1016/j.physbeh.2017.03.003 [Epub]
- Behrman RE, Kliegman R, enson HB. Nelson Textbook of Pediatrics, 16th edition ed: Behrman RE, Publisher: W B Saunders P. 1462, 2000.
- Braun MM, Barston CH, Pyzocha NJ. Diagnosis and management of sodium disorders: hyponatrimia and hypernatremia. Am Fam. Physician 1, 91(5):299-307. Mar 2015.
- Christensen, E. H. Physiological valuation of work in Nykroppa iron works. In: Fatigue, edited by Floyd, W. F. and Welford, A. T. London: H. K. Lewis. 1953.
- Clark, R. P., Human Skin temperature and connective heat loss. In: K. Eena and J.A. Clark (eds). Bioengineering, Thermal Physiology and Comfort. New York, N.Y.: Elsevier, pp 57 – 76; 1981.
- Epstein, Y. Shapiro, Y. and Brill, S. Comparison between different auxiliary cooling devices in a severe hot / dry climate. Ergonomics, 29, p. 41 – 48. 1986.
- Garrett AT, Goosens NG, Rehrer NJ, Patterson MJ, Harrison J, Sammut I, Cotter JD. Short-term heat acclimatization is effective and may be enhanced rather than impaired by dehydration. Am J. Hum Biol; 26 (3): 311 – 20, May-Jun 2014.
- Gerber GS, Brendler CB. Evaluation of the urologic patient: history, physical examination and urinalysis. In: Wein AJ, Kavoussi LR, Novick AC, et al. eds. Campbell – Walsh Urology. 10ed. Philadelphia, Pa Elsevier Saunders; chapter 3, 2011.
- Hahn G, Waldrens N, An aggregate urine analysis tool to detect acute dehydration. Int. J. Sports Nutr Exerc Metab. 23 (4): 303 – 11, Aug 2013
- Harrison, M. H., Edwards, P. A. Fennessy. Intravascular volume and tonicity as factors in the regulation of blood temperature. J. Appl. Physiol. 44: 69 – 75. 1978.
- Harrison, M.H., Edwards, R. J., Leitch, D. R. Effect of exercise and thermal stress on plasma volume. J. Appl. Physiol. 50: 597 – 604. 1981.
- Harrison, M. H.. Graveney, M. J., Cochrane, L. A. Some source of error in the calculation of relative change in plasma volume. Eur. J. Appl. Physiol. Occup. Physiol. 50: 13 – 21. 1982.
- Johnson, Kevin B. The Harriet Lane Handbook: A manual for Pediatric house officers, 13th edition / ed: Kevin B Johnson pg:231, Pub: Mosby c 1993.
- Jones B, Till K, King R, Gray M, O’hara J. Are habitual hydration strategies of female rugby league players sufficient to maintain fluid balance and blood sodium concentration during training and match – play? A research note from the field. J. Strength Cond Res; 30 (3): 875– 80, Mar 2016.
- Kamijo Y, Ikegawa S, Nose H. Mechanism of heat acclimatization with endurance training in humans: A role of Active Cutaneous Vasodilator. Japanese Journal of Physical Fitness and sports Medicine. Vol 61, No 3: 279 – 288. 2012
- Kenefick RW, Cheuvront SN. Physiological adjustments to hypohydration: Impact on thermoregulation. Auton Neurosci. 196: 47 – 51. April 2016.
- Ladell, W. S. S. Effects on man of restricted water supply. Brit. Med. Bull. 5.9 1947.
- Laxmi P S, Kapoor M, Singh SB. Heat: not black, not white. Its gray. Journal of Basic and Clinical Physiology and Pharmacology. Vol 24, Issue 4. Nov 2013.
- Maughan RJ, Meyer NL. Hydration during intense exercise training. Nestle Nutr Inst Workshop Ser; 76:25 – 37, 2013, Doi:10.1159/000350225 Epub-Jul2013
- RA, Ben Ezra J. Basic Examination of urine. In: McPhearson RA, Pincus MR. eds Henry’s Clinical Diagnosis and Management by Laboratory methods. 22nd ed. Philadelphia; Pa: Elsevier Saunders; Chapter 28; 2011.
- Medha K, Laxmi PS, Bajaj AC, Bharadwaj A, Chaudhary P, Gupta RK, Baburaj TP, Singh SB. The impact of exertional heat stress induced hypohydration on human cardiovascular function.
- Montain S. Latzka W. A. Sawka M. N. Fluid replacement recommendations for training in hot weather. Mil. Med; 164: 502 – 508. 1999.
- Patterson MJ, Stocks JM, Taylor NA. Whole body fluid distribution in humans during dehydration and recovery, before and after humid-heat acclimatization induced using controlled hyperthermia. Acta Physiol (Oxf); 210 (4):899 – 912. Apr 2014.
- Rogers R, Cole R. Hydration status in US military officer students. US Army Med Dep J.: 24-9; Jan – mar 2016.
- Rowell, L. B. Human Cardiovascular adjustment to exercise and thermal stress. Physiol. Rev. 54: 75 – 159, 1974.
- Saat M, Sirisinghe R G, Singh R and Tochihara Y. Effects of short term exercise in the heat on thermoregulation, blood parameters, sweat secretion and sweat composition of tropic dwelling subjects. J Physiol Anthropol Appl Human Sci, 24: 541 – 549, 2005.
- Tucker MA, Six A, Moyen NE, Satterfield AZ, Ganio MS. Effect of hypohydration on postsynaptic cutaneous vasodilation and sweating in healthy men. Am J Physiol. Regul Integr Comp Physiol 00525.2016. Feb 2017.
- Wilk B, Timmons BW, Baror O. Voluntary fluid intake, hydration status and aerobic performance of adolescent athletes in the heat. Appl. Physiol Nutri Metab; 35 (6): 834 – 41
- Yaglon, C.P., Minard, D. Control of heat casualties at military training centers. Arch. Industr. Hlth. 16, 302. 1957
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License