IJCRR - 4(18), September, 2012
Pages: 109-122
Date of Publication: 29-Sep-2012
Print Article
Download XML Download PDF
RELATIONSHIP OF LOWER LIMB SPASTICITY, STRENGTH AND GROSS MOTOR FUNCTION IN CHILDREN WITH SPASTIC DIPLEGIA: A CROSS-SECTIONAL STUDY
Author: Kamat PA , Ganesan S, Jaya Shanker Tedla
Category: Healthcare
Abstract:Purpose: To establish the relationship between spasticity and strength in the lower limb muscles and gross motor function of children with spastic diplegia. Method: This cross-sectional study included thirty children (21 males, 9 females) with spastic diplegia of GMFCS-EandR levels I to V between the age of 5 to 15 years. Spasticity, strength and gross motor function were assessed using tardieu scale, hand-held dynamometer and Gross Motor Function Measure respectively. Results: The correlation between spasticity, strength and gross motor function was analyzed using the spearman's correlation. A negative correlation was found between spasticity of hip flexors, hip adductors and knee extensors with GMFM. No correlation was found between spasticity and strength. A positive correlation was found between strength of hip abductor, knee flexors, dorsiflexors and plantarflexors with GMFM. Conclusion: Aggregate spasticity of muscles around the hip, knee and ankle joint showed a negative correlation with GMFM, whereas aggregate strength of muscles around all the 3 joints showed a positive correlation with GMFM. Hip flexor was the only muscle that showed a negative correlation between spasticity and strength.
Full Text:
INTRODUCTION
Cerebral palsy describes a group of disorders of the development of movement and posture, causing activity limitations that are attributed to non-progressive disturbances that occurred in the developing fetal or infant brain. The motor disorders of cerebral palsy are often accompanied by disturbances of sensation, cognition, communication, perception, behaviour or by a seizure disorder.1 Cerebral palsy (CP) has been generally classified on the basis of motor abnormalities as spastic, dyskinetic and ataxic.1 Based on the topographic distribution of impairments, spastic CP is divided into monoplegia, hemiplegia, diplegia, triplegia and quadriplegia.2 Spastic diplegia is the most common form of spastic cerebral palsy, occurring in 21.9 % of cerebral palsy children.2, 3 Children with spastic diplegia have many neurological deficits that interfere with motor function and daily activities. These impairments include neuromuscular and musculoskeletal problems such as spasticity, weakness, loss of selective motor control, incoordination and contractures.4 In children with spastic diplegia, lower limbs are more severely affected than upper limbs.2 Lower extremities exhibit abnormal timing of muscle contraction, poor ability to terminate muscle activity, and also show limited functional synergies and poor grading of co-contractions.5 Spasticity has been viewed as a major primary impairment of body function in spastic diplegics. Despite the lack of consensus on the role of spasticity in motor abilities, alleviations of spasticity remain the primary focus in the clinical management of spastic diplegics. Spasticity might produce contractures due to a marked loss of sarcomeres in the muscle, increase stiffness in the spastic muscle and changes connective tissues within the muscle. 4 Strength is an important aspect of normal motor control.6 Research finding indicate that children with spastic diplegia are indeed weak and that strength is directly related to motor function and therefore this weakness can be associated with difficulties in performing everyday functional activities.7 Gross motor development in children is commonly described as the acquisition of motor milestones such as unsupported sitting, crawling and walking. Children and infants with spastic diplegia are at risk for gross motor developmental disabilities. There is evidence that severity of the disorder is related to development of gross motor function. The primary goal of therapeutic intervention for children with spastic diplegia is to enhance the child’s ability to perform activities in the context of daily life. Relationship between motor impairments and functional activity has a significant impact on clinical practice.4, 8 Limited literature is available about the relationship of strength, spasticity, and gross motor function in children with spastic diplegia. The three variables of strength, spasticity and function have been correlated in various combinations at various times, but a general consensus regarding the relationship of the three has not been reached. The results of published literature shows high level of variation with some studies suggesting a significant relation between the three variables and many establishing insignificant or no relation.4,9-12 A study was done on children with spastic diplegia of GMFCS levels I to III to determine the relation between spasticity, strength, gross motor function and the functional measures of gait. They used Isokinetic dynamometer to measure spasticity and strength of selected ankle, knee and hip muscles. Gait analysis was done to evaluate linear and kinematic variables. They had also recorded gross motor function using GMFM 66. They concluded that spasticity did not account for a substantial amount of variance in gait and gross motor function. There was a moderate to high correlation between strength, gait linear data and gross motor function.10 Studies done on the relation between strength, spasticity, and gross motor function have used Isokinetic dynamometer to record strength or spasticity on children of GMFCS levels I to III. Most of the studies were done by either taking a single joint or all 3 joints of the lower limbor aggregate spasticity and aggregate strength.10, 11, 13 Isokinetic dynamometers are expensive instruments, requiring specific training for data collection and recording, which is usually provided by the manufacturers. This makes it inaccessible to many pediatric physiotherapy units. There are many cost effective, easy to perform reliable tools available for recording spasticity, strength and gross motor function like Tardieu, hand held dynamometer and GMFM-88 respectively.In children with spastic diplegia of GMFCS-EandR levels I to V, evidences regarding the relationship of spasticity, strength and gross motor functions are largely unknown. Studies regarding comparison of individual joint involvement with gross motor function are also limited. Aim of the current study was to establish the relationship between spasticity and strength in the lower limb muscles and gross motor function of the children with spastic diplegia of GMFCS-EandR levels I to V by using Tardieu scale, hand held dynamometer and GMFM-88 respectively. Objective of the study is to evaluate if individual joint involvement can have an effect on gross motor function of the children with spastic diplegia.
METHODOLOGY
This was a cross-sectional study using a convenient sampling method included 30 (21males and 9 females) children with spastic diplegia between the age of 5 to 15 years of GMFCS- EandR level I –V. These children were graded on Modified Child Mini Mental State Examination.19 Only those who had a minimum score of >24 for 5years, >28 for 6-8years, >30 for 9-11 years and >35 for 12-15 years were included. Those children who had an history of corrective surgeries, Botox / phenol injections within the past 6 months, any systemic or musculoskeletal disorders interfering with performance of child, children who are taking muscle relaxants (baclofen, dantrolene), or those who had fixed flexion contracture of hip and knee >25° and fixed ankle plantarflexion contracture of > 10° were excluded. The materials used were GMFCS-EandR, GMFM-88 scale, Baseline pushpull digital TM dynamometer, Tardieu scale, Omega Universal Goniometer.
Procedure
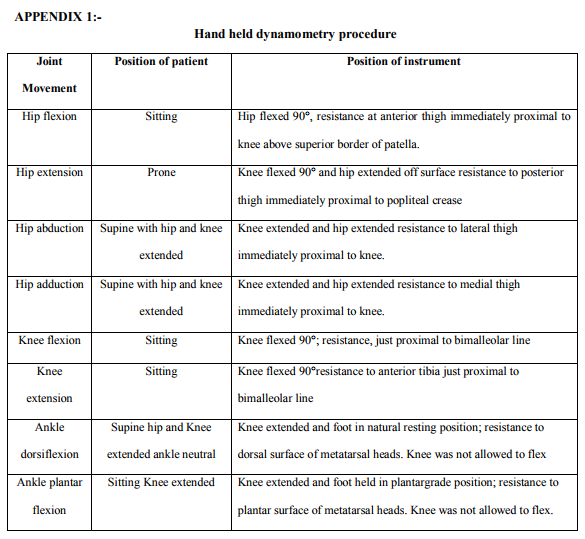
Approval from the scientific committee and time bound research ethics committee was obtained prior to commencement of the study. All parents of the children with spastic diplegia signed the consent form. Children aged 8 years and above signed the assent form. Children of both genders diagnosed by pediatrician as spastic diplegics were screened by the tester for inclusion and exclusion criteria. Children who fulfilled the inclusion criteria wereclassified on the GMFCS-EandR levels I toV.16, 23 Spasticity, strength and gross motor function was assessed using the Tardieu scale, hand held dynamometer and GMFM-88 respectively. In children with spastic diplegia the spasticity and strength of hip flexors, extensors, adductors and abductors, knee flexors, and extensors, ankle dorsiflexors and plantarflexors of both lower limbs were tested using Tardieu scale20,21,25 and hand held dynamometer14,26,32 respectively. Spasticity was assessed in one attempt only. The hand-held dynamometer was used to quantify isometric strength of the major lower extremity muscle groups bilaterally. Children were positioned in the respective test positions (Appendix-1). The proximal joint segment was stabilized. The plate of the dynamometer was then placed distally on the distal joint segment. The piston of the dynamometer was held perpendicular to the limb segment in the direction of the movement to be performed. The subject was then asked to produce a maximal isometric contraction of the muscle group, tested by pushing against the plate of the dynamometer and holding in position for duration of 1 second to allow the participant to adjust and recruit the maximum number of muscle fibers. Three attempts were recorded. 1st attempt was to familiarize the child with the test procedure and the final reading was obtained from the best out of the 2nd and 3rd readings. The Gross Motor Function Measure (GMFM)was administered to measure gross motor function quantitatively. The GMFM consists of 88 items grouped into 5 dimensions: (1) lying and rolling (2) sitting, (3) crawling and kneeling (4) standing and (5) walking, running, and jumping.17
Data Analysis
The values of spasticity and strength of hip flexors, extensors, adductors and abductors, knee flexors and extensors, ankle dorsiflexors and plantarflexors between right and left side were compared by using Mann-Whitney U test. The data of spasticity and strength of hip flexors, extensors, adductors and abductors, knee flexors and extensors, ankle dorsiflexors and plantarflexors and gross motor function was analyzed using the spearman’s correlation. pvalue< 0.05 was considered significant at 95% confidence interval. SPSS-13 version was used for analysis.
RESULTS
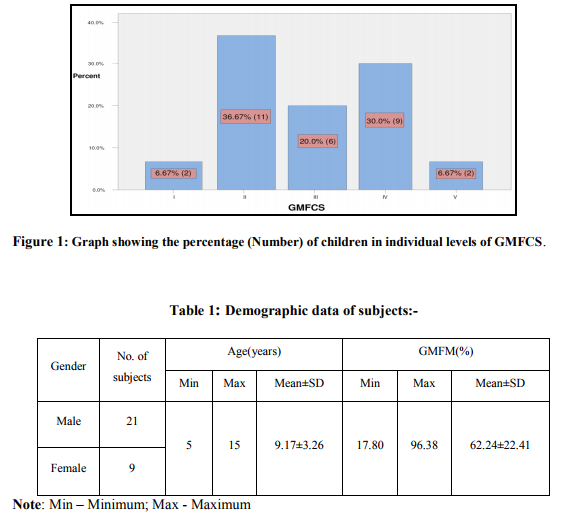
The aim of this study was to establish a relationship between spasticity, strength and gross motor function in children with spastic diplegia between the age group of 5 to 15 years. The subjects were classified on the gross motor function classification system levels I to V. The total number of children included in the study was 30, out of which 21 were males and 9 were females. The demographic data such as age and gender was obtained. The number of subjects mean and standard deviation of their age and GMFM scores is shown in table1 and figure 1. The comparison of spasticity and strength between the right and left sides showed that there was no significant difference in spasticity and strengthof hip flexors, extensors, adductors and abductors, knee flexors and extensors, ankle dorsiflexors and plantarflexors between the right and left side. Thus as observed that there was no significant difference in spasticity and strength of hip flexors, extensors, adductors and abductors, knee flexors and extensors, ankle dorsiflexors and plantarflexors between the right and left side.Therefore, the values of spasticity and strength of individual muscles of right and left side was added together for the purpose of correlation analysis between spasticity, strength and gross motor function. In addition, the aggregate values of spasticity and strength of each joint as a whole of right and left side together was correlated with gross motor function.
A. Correlation between spasticity, strength of muscles around the hip jointand gross motor function.
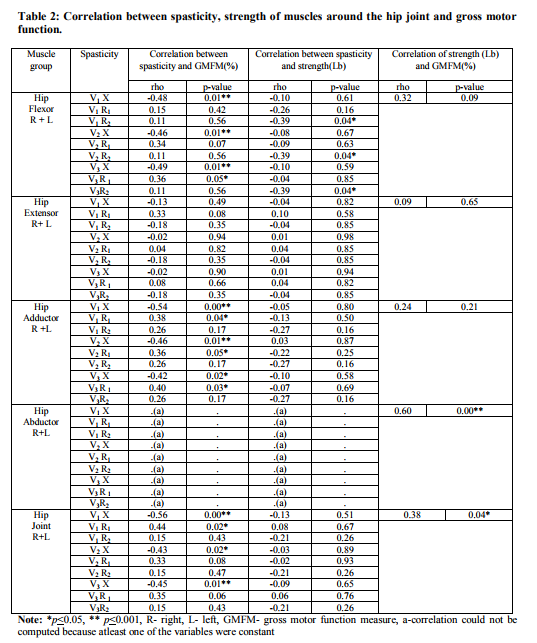
Correlation of spasticity and strength of muscles around the hip joint and gross motor function was done using the spearman’s correlation coefficient as shown in table 2 Correlation between Spasticity and GMFM As shown in table 2, there was a negative correlation of quality of muscle reaction of hip flexors and adductors, and positive correlation of angle of muscle reaction of hip flexors and adductors with GMFM. There was no correlation between the quality and angle of muscle reaction of hip extensors and abductors with GMFM. When aggregate spasticity of muscles around the hip joint was considered, there was negative correlation between quality of muscle reaction and positive correlation between angle of muscle reaction with GMFM as shown in table 2. Correlation between Spasticity and Strength The quality of muscle reaction of the hip flexor spasticity showed no correlation with strength but the angle of muscle reaction of hip flexors showed negative correlation with strength. There was no correlation between the quality and angle of muscle reaction of the hip extensors, adductors and abductors, and the aggregate hip joint with strengthas shown in table 2.
Correlation between Strength and GMFM
There was no correlation between the strength of hip flexors, extensors and adductors with GMFM. There was a significant positive correlation of hip abductor and the aggregate hip joint strength with GMFM as shown in table 2.
B. Correlation between spasticity, strength of muscles around the knee joint and gross motor function.
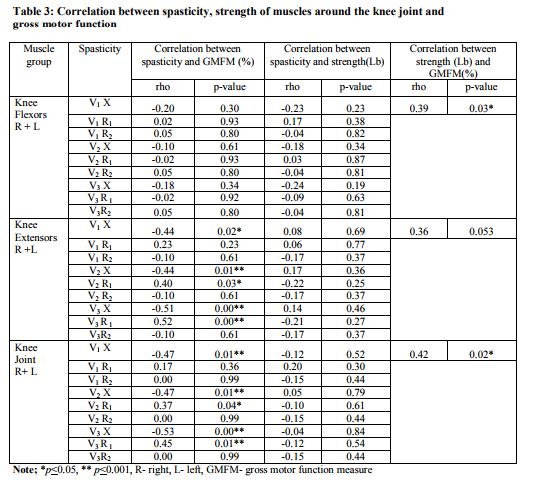
Correlation of spasticity and strength of muscles around the knee joint and gross motor function was done using the spearman’s correlation coefficient as shown in table 3. Correlation between Spasticity and GMFM As shown in table 3 there was no correlation between quality and angle of muscle reaction of knee flexors with GMFM.There was a negative correlation between the quality of muscle reaction of the knee extensors, and the aggregate of knee joint with GMFM and a positive correlation of the angle of muscle reaction of knee extensors and aggregate of knee joint with GMFM. Correlation between Spasticity and Strength There was no correlation between quality and angle of muscle reaction of the knee flexors, knee extensors and aggregate knee joint with its strength as shown in table 3 Correlation between Strength and GMFM There was a positive correlation between strength of knee flexors, and aggregate knee joint with GMFM. Strength of knee extensors had no correlation with GMFM as shown in table 3.
C. Correlation between spasticity, strength of muscles around the ankle joint and gross motor function
Correlation of spasticity and strength of muscles around ankle joint and gross motor function was done using the spearman’s correlation coefficient as shown in table 4. Correlation between Spasticity and GMFM As shown in table 4 there was no correlation in quality and angle of muscle reaction of ankle dorsiflexors with GMFM. There was a positive correlation between angle of muscle reaction of plantarflexors and aggregate ankle joint, and a negative correlation between the quality of muscle reaction of the aggregate ankle joint with GMFM. Correlation between Spasticity and Strength There was no correlation of quality and angle of muscle reaction of dorsiflexors, plantarflexors and aggregate ankle joint with its strength as shown in table 4. Correlation between Strength and GMFM There was positive correlation of strength in dorsiflexors, plantarflexors and aggregate ankle joint with GMFM as shown in table 4.
DISCUSSION
The aim of the current study was to establish a relationship between spasticity, strength and gross motor function of children with spastic diplegia of GMFCS-EandR levels I to V and to evaluate if individual joint involvement can have an effect on gross motor function. The spasticity was tested using the Tardieu scale, strength using the hand held dynamometer and gross motor function using the GMFM-88. The study included 30 children (21 males and 9 females) with a mean age of 9.17±3.26 years. Correlation between Spasticity and GMFM The results of the present study showed that the quality of muscle reaction of the hip flexors and adductors, knee extensors and aggregate of hip, knee and ankle was negatively correlated with the gross motor function. This shows, when spasticity is less, the level of gross motor function is high. In children with spastic diplegia, the spasticity in the lower extremities causes use of limited synergies in all function i.e. they have poor ability to grade co-contraction, reciprocal inhibition, terminate sustained muscle activity and abnormal timing of muscle contraction. In addition to these, there is rapid development of secondary impairments in the musculoskeletal system leading to shortened muscles, mal-aligned jointsand deformed bones. Shortening of hip flexors, adductors and medial hamstrings leads to hip flexion, adduction and internal rotation posture which narrows the base of support in all positions, and makes learning upright trunk control more difficult. When the flexion component is stronger than the internal rotation component, the rectus femoris exerts a strong influence as hip flexors and knee extensor leading to extended knees.5,9,27,33 Our results were supported by a report of Tuzson et al. who determined a spastic threshold velocity, using electromyography during isokinetic testing, for the quadriceps and hamstrings and found it moderately correlated with the Gross Motor Function Measure (GMFM) walk and run domain (r =.58) and walking velocity (r =.64), indicating the milder the spasticity, the higher the function.27 The ankle mostly assumes a plantarflexed position, because of the large cross-sectional area of the plantarflexors compared to the dorsiflexors. Functionally the child is limited to the use of hip flexion, adduction, internal rotation and ankle plantarflexion with variable knee positions. This leads to lack of variety of movement which is essential for gross motor function. Thus, when spasticity in certain muscle groups is high the gross motor function is reduced.4, 5 Correlation between Spasticity and Strength The results of the present study showed that the quality and angle of muscle reaction of hip extensors, adductors and abductors, knee flexors and extensors, ankle dorsiflexors and plantarflexors, had no correlation with strength except the angle of muscle reaction of hip flexor which was negatively correlated with strength.
The negative correlation between spasticity and strength of hip flexors could be because typically children with spastic diplegia use the superficial lumbar extensors with the hip flexors as prime movers or in synergy to control the upper trunk on the pelvis. As these children also have loss of selective motor control, so whenever there is a voluntary contraction of the muscles, the lumbar spine goes into end- range extension with some degree of hip flexion leading to overlengthened abdominal muscles further weakening their use. This repeated use of hip flexors which causes an increase in their strength and, therefore leads to a decrease in the spasticity. This was supported by Morton et al who reported that with an increase in the muscle strength there is decrease in the spasticity. This explains the negative correlation between spasticity and strength.5, 11, 28, 29 Correlation between strength and GMFM There was positive correlation between strength of hip abductors, knee flexors, ankle dorsiflexors and plantarflexors and aggregate hip, knee and ankle joint with GMFM. Hip abductors strength in children with CP has been reported to be significantly less than the typically developing children.Hip abductor strength is important for kneel and half kneel skills, single-limb balance, and gait. Weak hip abductors will result in a contralateral pelvic drop and excessive hip adduction during gait. In the present study, the hip abductor strength appeared to be most closely correlated to gross motor function than any other lower-extremity muscle group.5, 7, 10, 24 In the present study, there was a positive correlation between strength of knee flexors and GMFM. Most of the children with spastic diplegia have a crouched posture due to inability to terminate the hamstrings. Over a period, this constant over activity leads to shortening of hamstrings causing inefficient muscle strength and decrease in knee extension ranges. Most of the components of GMFM requires synergistic action of muscles across the joints with normal timing of contraction and graded control which becomes difficult with abnormal alignment because of the short hamstrings. This can explain the positive correlation of knee flexors and GMFM.5, 7, 18, 24 Strength of ankle dorsiflexors showed a highly significant correlation with gross motor function. This could be because children with spastic diplegia experience varying degree of reduced motor control of their distal musculature which compromises their ability to dorsiflex their feet. This presents a significant problem for many children as it impedes a normal heel strike during gait, forcing children to walk on toes. Various mechanisms contribute to reduced dorsiflexion including altered neural control, increased stiffness of the plantarflexors or weakness of dorsiflexors. 5, 15, 30 Similarly even plantarflexors showed positive correlation to gross motor function. Like the hamstrings, the plantarflexors are also overactive, leading to shortening and inability to move ankle joint effectively during functional activities. This weakness in ankle dorsiflexors and over activity in plantarflexors leads to inefficient co-contraction or timing causing reduction in standing and walking function. These results were similar to the study done by Ross et al who reported that increase in ankle strength improved gross motor function.6, 15, 31 In the present study a positive correlation was found between strength of hip abductors, ankle dorsiflexors and plantarflexors. Similar results have been shown in a previous study done by Ross et.al on relationship between spasticity, strength, gross motor function and gait in children with spastic diplegia. This study reported that strength was positively correlated with gross motor function in hip abductors, ankle dorsiflexors and plantarflexors.10 Subgroup analysis of relationship between spasticity, strength and gross motor function of children in the different levels of GMFCS was not done due to insufficient sample size in each level.
Psychometric properties of Tardieu scale in hip flexors, extensors, and abductors, knee extensors, have not been established. A single observer assessed all the children on the Tardieu scale, hand-held dynamometer and GMFM. This may have affected the results in the present study. Further studies can be done to find out relationship between spasticity, strength and gross motor function in other types of cerebral palsy and in different levels of GMFCS levels may be established.
CONCLUSION
In the relationship between spasticity and GMFM, there was a significant negative correlation between aggregate spasticity of muscles around the hip, knee and ankle joint and the gross motor function. But when individual muscle analysis was done only hip flexors, adductors and knee extensors showed negative correlation with gross motor function. In the relationship between strength and GMFM, a significant positive correlation was found between aggregate strength of muscles around the hip, knee and ankle joint and the gross motor function. But when individual muscle analysis was done only strength of hip abductors, knee flexors, ankle dorsiflexor and plantarflexors showed positive correlation with gross motor function. In the relationship between spasticity and strength, the spasticity of hip flexors were the only muscles that showed a negative correlation with strength, where as spasticity of other muscles showed no correlation with strength.
ACKNOWLEDGEMENT
Authors acknowledge the immense help received from the scholars whose articles are sited and included in references of this manuscript. the authors are also grateful to authors/ editors/ publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
References:
1. Goldstein M, Bax M, Rosenbaum P, Leviton A, Paneth N. Proposed definition and classification of cerebral palsy april 2005. Dev Med Child Neurol 2005;47:571-6.
2. Shankar C, Mundkur N. Cerebral palsy – definition, classification, etiology and early diagnosis. Indian J of Pediatr 2005;72:865-8.
3. Srivastava VK, Laisram N, Srivastava RK. Cerebral palsy. Ind Pediatr 1992;29:993-6.
4. Carlberg EB, Ostensj O S, Vollestad NK. Motor impairment in young children with cerebral palsy, relationship to gross motor function and everyday activities. Dev Med Child Neurol 2004;46:580–9.
5. Stamer M. Posture and movement of the child with cerebral palsy. USA. Therapy skill builders; 2000. Chapter 4, Children with hypertonia; p.104 -24.
6. Dodd KJ, Taylor NF, Graham H. A randomized clinical trial of strength training in young people with cerebral palsy. Dev Med Child Neurol 2003;45:652–7.
7. Damiano D, Abel MF. Functional outcome of strength training in spastic cerebral palsy. Arch Phys Med Rehab1998;79:119-25.
8. Hanna SE, Palisano RJ, Rosenbaum PL, Russell DJ, Walter SD, Wood EP, Raina PS, Galuppi BE. Validation of a model of gross motor function for children with cerebral palsy. Phys Ther 2000;80:974-85
9. Gorter JW, Verschuren O, Riel LV, Ketelaar M. The relationship between spasticity in young children {18 months of age} with cerebral palsy and their gross motor function development.BMC Musculoskeletal Disorder 2009;10:108-16.
10. Ross SA, Engsberg JR .Relationship between spasticity, strength, gait, and the GMFM-66 in person with spastic diplegic cerebral palsy. Arch Phys Med Rehab.2007;88:1114-20 .
11. Damiano DL, Quinlivan J, Owen BF, Shaffrey M, Abel MF. Spasticity versus strength in cerebral palsy: relationships among involuntary resistance, voluntary torque, and motor function. Eur J Neurol 2001;8:40-9.
12. Eek MN .Muscle strength, gross motor function and gait pattern in children with cerebral palsy. Institution of clinical science \ Department of pediatrics at Schlgrenska academy, University of Gotherberg - 2009 – unpublished thesis
13. Eeka MN, Eva B. Walking ability is related to muscle strength in children with cerebral palsy. Gaitpost 2008;28:366-71 14. Crompton J, Galea MP, Phillip B. Hand held dynamometer for muscle strength measurement in children with cerebral palsy. Dev Med Child Neurol 2007;49:106 –11.
15. Engsberg JR, Ross SA, Collins DR. Increasing ankle strength to improve gait and function in children with cerebral palsy: A pilot study. Pediatr Phys Ther 2006;18:266-75.
16. Palisano R, Rosenbaum P, Bartlett D, Livingston M. Content validity of the expanded and revised Gross Motor Function Classification System. Dev Med Child Neurol 2008;50:744-50
17. Russell D.J., Rosenbaum P.L., Avery L.M., Lane M. Gross Motor Function Measure (GMFM-66 and GMFM-88) user’s manual. New Jersey: Wiley Black Well publishers: 2002
18. Damiano D, Kelly LE, Vaughn CL. Effect of quadriceps femoris muscle strengthening on rouch gait in children with spastic diplegia. Phys Ther 1995;75:658-67
19. Jain, Passi GR. Assessment of a Modified mini mental scale for cognitive function in children Ind Pediatr 2005;288:1357– 63.
20. Vanessa A, Scholtes B, Becher GJ, Lankhorst G J. Clinical assessment of spasticity in children with cerebral palsy, a critical review of available instrument. Dev Med Child Neurol 2006;48:64-73.
21. Gracies JM, Clegg NJ, Browne R, Rushing C, Fehlings D, et al. Reliability of the Tardieu scale for assessing spasticity in children with cerebral palsy. Arch Phys Med Rehabil 2010;91:421-8
22. Russell DJ, Avery LM, Rosenbaum PL, Raina PS, Walter SD, Palisano RJ. Improved scaling of the gross motor function measure for Children with cerebral palsy: evidence of reliability and validity. Phys Ther 2000;80:873-85.
23. Palisano R, Rosenbaum P, Bartlett D, Livingston M. GMFCS – E and R Gross Motor Function Classification System Expanded and Revised. Downloaded from can child website at: http://motorgrowth.canchild.ca/en/GMFCS/res ources/GMFCS-ER.pdf
24. Eek MN, Tranberg R, Zugner R, Kristina A, Eva B. Muscle strength training to improve gait function in children with cerebral palsy. Dev Med Child Neurol 2008;50:759-64.
25. Haugh AB, Pandyan AD, Johnson GR. A systematic review of the tardieu scale for the measurement of spasticity.Disability and Rehabilitation 2006;28:899-907
26. Eek MN, Kroksmark Ak, Beckung E. Isometric Muscle Torque in Children 5 to 15 Years of Age: Normative Data. Arch Phys Med Rehabil 2006;87:1091-9.
27. Tuzson AE, Granata KP, Abel MF. Spastic velocity threshold constrains functional performance in cerebral palsy. Arch Phys Med Rehabil 2003;84:1363–8.
28. Ross SA, Engsberg JR. Relation between spasticity and strength in individual with spastic diplegic cerebral palsy. Dev Med Child Neurol 2002;44:148 –57.
29. Morton JF, Brownlee M, McFadyen AK. The effects of progressive resistance training for children with cerebral palsy. Clin Rehabil 2005;19:283-9.
30. Tecklin JS, Pediatric Physical Therapy, 4 thedition USA: Lippincott Williams and Wilkins; 2008. Chapter 5, The infant and child with cerebral palsy; p. 179-230.
31. Wiley ME, Damiano DL. Lower extremity strength profile is spastic cerebral palsy. Dev Med Child Neurol 1998;40:100-7.
32. Taylor NF, Dodd KJ, Graham HK .Test retest reliability of hand held dynamometer strength testing in young people with cerebral palsy. Arch Phys Rehabil 2004;85:77-80.
33. Ohata K, Tsuboyama T, Haruta T, Ichihashi N, Kato T, Nakamura T. Relation between muscle thickness, spasticity, and activity limitations in children and adolescents with cerebral palsy. Dev Med Child Neurol 2008;50:152–56
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License